Asthma: Overview
Asthma is a chronic lung disease which causes wheezing, coughing, and breathing difficulty.
- check your overall health status
- understand what's happening to your body
- have a doctor review your case (optional)
Asthma can be managed but not cured. It causes the airways to become very sensitive and to react to contact with a variety of airborne substances. A severe asthma attack can be a traumatic – or even life-threatening – experience.
Incidence; Causes and Development
Although asthma occurs at all ages, it is most common in children under 10. There is a 2:1 male:female ratio in children, which equalizes by the age of 30.
Mild episodic asthma is mainly due to bronchial smooth muscle contraction whereas moderate to severe sustained asthma is largely due to chronic inflammation of the bronchi with the presence of white cells such as eosinophils, neutrophils and mononuclear cells that are part of an inflammatory response. These cells contribute products that inflame the airways.
People with asthma have airways that are super-sensitive to 'triggers' that do not bother people without asthma. When an asthmatic is near to or comes in contact with a trigger, an asthma episode (asthmatic attack) may start. The airways and their linings may become swollen, produce mucus, and tighten up. The muscles around the airways can also tighten, making the airways even narrower. As the airways narrow, breathing becomes more difficult.
Common triggers for asthma episodes include the following:
- Dander (or flakes) of skin, hair, or feathers of all warm-blooded pets
- House dust mites
- Cockroaches
- Pollens from grass and trees
- Molds (indoor and outdoor)
- Cigarette smoke or wood smoke; scented products such as hair spray, cosmetics, and cleaning products; strong odors from fresh paint or cooking; automobile fumes; and air pollution
- Infections in the upper airway, such as colds (a common trigger for both children and adults)
- Exercise
- Expressing strong feelings (crying, laughing)
- Changes in weather and temperature
Signs and Symptoms
Asthmatic attacks often occur at night or early in the morning. Symptoms can be mild, moderate or severe and life-threatening.
During an attack, an asthmatic trigger causes the airway walls to swell, and the muscles around the airways to contract. The airways narrow, and breathing through them produces a whistling sound (wheezing). Mucus is produced by the lining of the airways, and this further clogs up the already-narrowed airways, making normal breathing more difficult.
Treatment and Prevention
The narrowing of the airways is reversible if the trigger is removed or if the inflammation is treated medically. Some medicines relax the airways while others reduce or prevent the inflammation, swelling and mucus. Natural methods of asthma management should be tried prior to, or along with, conventional treatments if possible.
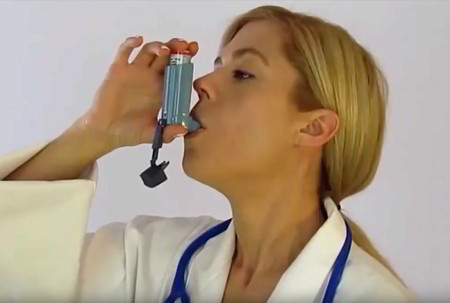
Inhaled bronchodilators and corticosteroids are a potent and consistently effective treatments for the inflammation of asthma. Metered dose inhalers (MDI) deliver a precise amount of medication, but they must be used correctly in order to deliver enough medication to the lungs to control symptoms:
- Remove the inhaler cap
- Hold it upright between thumb and middle finger
- Shake it several times to mix the contents
- Tilt head slightly back to open airways
- Breathe out
- Place the inhaler between the teeth and grip with the lips to form a seal
- Start to breathe in slowly for 3-5 seconds while pressing down on the inhaler
- Hold breath for 10 seconds to let the medicine take effect
- Start breathing normally
- Repeat if necessary, waiting 1 minute between puffs
Salbutamol inhalers are safe and effective with few side-effects when used properly. They provide quick relief from breathing problems as required, and can also be used for prevention. Salbutamol is safe to use during pregnancy and breastfeeding. Common brand names for salbutamol inhalers include Ventolin, Airomir, Easyhaler, Salamol Easi-Breathe and Salbulin.
Other types of inhaler include MDI with a Spacer to reduce throat irritation, and breath-activated dry powder inhalers.
Seek medical attention if...
Talk to a doctor if you need to use your inhaler more than 3 times a week because that may be a sign that your breathing problem is not well controlled.
Signs, symptoms & indicators of Asthma:
Lab Values - Cells
Symptoms - Environment
 Difficulty breathing in cold weather
Difficulty breathing in cold weather
Asthma attacks are usually triggered by the body's response to an allergy, but inhaling cold air can also trigger bronchospasms.
 Breathing unaffected by cold weather
Breathing unaffected by cold weather
Asthma attacks are usually triggered by the body's response to an allergy, but inhaling cold air can also trigger bronchospasms.
Symptoms - Respiratory
 Occasional/regular chest tightness
Occasional/regular chest tightness
As the airways become inflamed and filled with mucus, and the smooth muscles in the airways constrict, chest tightness may be experienced as the feeling of not being able to move air in and out of the lungs. This feeling may in turn increase anxiety, which worsens the feeling of tightness. These may occur after exposure to a trigger, or a specific irritant, or after exercise.
 Recent/chronic productive cough
Recent/chronic productive cough
Not all people with asthma wheeze. For some, chronic coughing, which often occurs during the night or after exercise, may be the only symptom.
Symptoms - Sleep
Conditions that suggest Asthma:
Dental / Oral
 Bruxism (Clenching/Grinding Teeth)
Bruxism (Clenching/Grinding Teeth)
Allergy may play a role in bruxism. It is noticed that bruxism is more frequent in those experiencing periods of allergic rhinitis or asthma.
Symptoms - Respiratory
Risk factors for Asthma:
Childhood
 Past vaccinations
Past vaccinations
Findings from animal and human studies confirm that DTP (diphtheria and tetanus toxoids and pertussis) and tetanus vaccinations can induce allergic responses [1, 2, 3, 4, 5] and can increase the risk of allergies, including allergic asthma. An analysis of data from nearly 14,000 infants and children revealed that having a history of asthma is twice as great among those who were vaccinated with DTP or tetanus vaccines than among those who were not [6].
[1] Vaccine 1995;13: pp.669-73
[2] Pediatr Allergy Immunol 1997;8: pp.83-7
[3] Pediatr Allergy Immunol 1994;5: pp.118-23
[4] Adv Immunol 1996;61: pp.341-403 [review]
[5] J Allergy Clin Immunol 1974;54: pp.25-31
[6] J Manipulative Physiol Ther 2000;23: pp.81-90
Mental
Metabolic
 Problems Caused By Being Overweight
Problems Caused By Being Overweight
Being overweight increases the risk of asthma. [Arch Intern Med 1999;159: pp.2582-8] Obese people with asthma may improve their lung-function symptoms and overall health status by engaging in a weight-loss program. A controlled study found that weight loss resulted in significant decreases in episodes of shortness of breath, increases in overall breathing capacity, and decreases in the need for medication to control symptoms. [BMJ 2000;320: pp.827-32]
Nutrients
 Selenium Requirement
Selenium Requirement
Dietary consumption of apples and selenium intake (assessed by food frequency questionnaire) were each associated with a reduced risk of asthma in an English study of adults. [Am J Respir Crit Care Med 2001;164(10): pp.1823-28]
Symptoms - Environment
 High air pollution exposure
High air pollution exposure
The number of people with asthma and the death rate from this condition have been increasing rapidly since the late 1980s. Environmental pollution may be one of the causes of this growing epidemic. Work exposure to flour or cotton dust, animal fur, smoke, and a wide variety of chemicals has been linked to increased risk of asthma. [Blanc PD, Eisner MD, Israel L, Yelin EH. The association between occupation and asthma in general medical practice. Chest 1999;115: pp.1259-64]
Symptoms - Muscular
 Being lean or underweight or being very skinny
Being lean or underweight or being very skinny
Slender, older women are more susceptible to various chronic lung problems such as bronchitis, pneumonia and asthma.
Asthma suggests the following may be present:
Allergy
 Allergy to Foods (Hidden)
Allergy to Foods (Hidden)
Asthma is one of the three manifestations of a pattern of allergy that is called atopy – a genetic tendency to develop allergic diseases. The other two are eczema and hay fever. Asthma due to allergy can come from both airborne and food sources. Patients with delayed pattern food allergy have the most severe and persistent inflammatory form of chronic asthma.
While airborne problems are more obvious to asthmatic sufferers, food problems may be a well-hidden source of lung disease. Many studies of food allergy involve patients with food-induced asthma. Eczema and asthma are often associated in atopic patients with food allergy.
In a group of 320 children with atopic dermatitis, 55% had asthma. Food challenges triggered respiratory symptoms in 59% (rhinitis, laryngeal edema, wheezing, and dyspnea). Asthma is frequently treated only as an airborne allergy problem or as a problem unrelated to allergic processes and the possible role of food allergy is neglected. It is overlooked because the usual skin tests are often negative and the history is often not helpful as symptoms appear gradually, hours or days after ingestion of the food. Milk, wheat, egg, yeast, preservatives, colorings, coffee and cheese are the main foods implicated.
Food allergens may be found in the bloodstream within circulating immune complexes that trigger the release of immune mediators into the bloodstream. These chemicals cause a variety of symptoms, including constriction of the bronchial smooth muscle in the lungs; this is the first event during an asthmatic attack. Airflow is reduced in the narrowed tubes. Air has a harder time leaving the lungs than entering, with the result of prolonged noisy exhalation. This inflammatory, obstructive phase is the most important mechanism of chronic asthmatic bronchitis.
Diet
Inflammation
 Chronic Inflammation
Chronic Inflammation
Asthma is simply a chronic inflammatory condition of the airways rather than some other part of the body, such as the joints. People with asthma have inflamed, hyperreactive airways that produce excessive bronchial mucus.
Nutrients
 Vitamin B6 Requirement
Vitamin B6 Requirement
Children with asthma have been shown to have a metabolic defect in tryptophan metabolism. Tryptophan is converted to serotonin, a known bronchoconstricting agent in asthmatics. Studies have shown that patients benefit from either a tryptophan-restricted diet or B6 supplementation to correct the blocked tryptophan metabolism. Pyridoxine may also be of direct benefit to asthmatic patients, since it is a key cofactor in the synthesis of all the major neurotransmitters.
Recommendations for Asthma:
Botanical / Herbal
 Ephedra (Ma Huang)
Ephedra (Ma Huang)
Ephedra contains ephedrine and variable quantities of pseudoephedrine. These components are still widely prescribed and effective drugs in the treatment of asthma, particularly in chronic cases.
Ephedrine is an approved over-the-counter (OTC) treatment for bronchial tightness associated with asthma. OTC drugs containing ephedrine can be safely used by adults in the amount of 12.5 to 25mg every four hours. Adults should take a total of no more than 150mg every 24 hours and refer to labels for children's dosages. Ephedra sinica continues to be a component of traditional herbal preparations for asthma, often in amounts of 1 to 2gm of the herb per day.
 Licorice Root
Licorice Root
Glycyrrhizin, found in licorice root, shows steroid-like activity and has a long history of use as an anti-inflammatory and anti-allergic agent, actions which have now been documented. Glycyrrhiza is an expectorant, which can be useful for relieving asthma.
 Cayenne Pepper
Cayenne Pepper
Capsaicin, cayenne pepper's major active component, induces long-lasting desensitization of airway linings to various mechanical and chemical irritants. This effect is probably due to capsaicin-induced depletion of substance P in the respiratory tract nerves. The respiratory and gastrointestinal tracts contain neurons which have large numbers of substance P receptors. Depletion of substance P may be desirable in asthma.
 Coleus
Coleus
A small double-blind trial found that inhaled forskolin could decrease lung spasms in asthmatics. [Clin Pharmacol Ther 1993;43: pp.76-83] It is unclear if oral ingestion of coleus extracts will provide similar benefits.
 Ivy Leaf
Ivy Leaf
A controlled trial in a group of children with bronchial asthma found that 25 drops of ivy leaf extract given twice per day was effective in improving airflow into the lungs after only three days of use. [Münch Med Wschr 1998;140: pp.32-6] However, the incidence of cough and shortness of breath symptoms did not change during the short trial period.
Standardized ivy leaf extract can be taken by itself or in water at 25 drops twice per day as a supportive treatment for children with asthma. [Giornale Italiano de Dermatologia Venereologia 1993;128; pp.619-24] At least double this amount may be necessary to benefit adults with asthma.
 Tylophora
Tylophora
One clinical trial with asthma sufferers found that tylophora leaf (150mg of the leaf by weight) chewed and swallowed daily in the early morning for six days led to moderate to complete relief of their asthma symptoms. [J Allergy 1969;43: pp.145-50] In a follow-up trial with asthma patients, an alcoholic extract of crude tylophora leaves in 1gm of glucose had comparable effects to that of chewing the crude leaf. [Ann Allergy 1972;30: pp.407-12]
Another trial found similar success in reducing asthma symptoms using a tylophora leaf powder at 350mg per day. [J Indian Med Assoc 1978;71: pp.172-6] However, the tylophora was not as effective as a standard asthma drug combination. One double-blind trial failed to show any effect on asthma for tylophora. [Ind J Med Res 1979;69: pp.981-9]
Tylophora leaf at 200-400mg of the dried leaf per day or 1-2ml of tincture per day can be used to treat asthma. [Clinical Applications of Ayurvedic and Chinese Herbs. Warwick, Queensland, Australia: Phytotherapy Press, 1996: pp.134-6]
 Picrorhiza
Picrorhiza
Two open-label, non-placebo, controlled human studies have shown picrorhiza to be of benefit in asthma. [Indian J Pharmacol 1975;7: pp.95-6, J Postgrad Med 1977;23: pp.118-20] However, a follow-up double-blind study did not confirm these earlier findings. [J Postgrad Med 1983;29: pp.89-95]
Diet
 Plant-Based Nutrition
Plant-Based Nutrition
A long-term trial of a vegan diet (elimination of all animal products) provided significant improvement in 92% of the 25 patients who completed the study. Drinking water was limited to spring water (chlorinated tap water was prohibited), and coffee, tea, chocolate, sugar and salt were excluded. [Journal of Asthma 1985; 22:44, p.13]
 Food Additive Avoidance
Food Additive Avoidance
The elimination of food additives is important in the control of asthma. Some asthmatics react to additives such as sulfur dioxide, tartrazine (yellow dye #5), and sodium benzoate, as well as natural salicylates (aspirin-like substances found in many foods). [J Asthma 1985;76: pp.40-5, Pediatrics 1984;73: pp.631-7] Sulfites in particular have been reported to cause asthma attacks in susceptible individuals. A doctor or an allergist can help determine whether chemical sensitivities are present.
 Increased Fruit/Vegetable Consumption
Increased Fruit/Vegetable Consumption
Vitamin C, present in fruits, is a powerful antioxidant and anti-inflammatory agent. Its anti-inflammatory activity may decrease the incidence of asthma symptoms. A large preliminary study has shown that young children with asthma experience significantly less wheezing if they eat a diet high in fruits rich in vitamin C.
Dietary consumption of apples and selenium intake (assessed by food frequency questionnaire) were each associated with a reduced risk of asthma in a case-control study (607 cases and 864 controls) of adults aged 16-50 in England. [Am J Respir Crit Care Med 2001;164(10): pp.1823-8]
 Elimination Diet
Elimination Diet
Although most people with asthma do not suffer from food allergies [J Asthma 1991;28: pp.5-9], unrecognized food allergy can be an exacerbating factor. [JAMA 1959;169: p.1158] A medically supervised allergy elimination diet followed by reintroduction of the eliminated foods, often helps identify problematic foods. A healthcare professional must supervise this allergy test because of the possibility of triggering a severe asthma attack during the reintroduction. [N Engl J Med 1992;327: pp.380]
 Alcohol Consumption
Alcohol Consumption
Red wine intake was associated with reduced asthma severity in a study of adults in England. [Am J Respir Crit Care Med 2001;164(10): pp.1823-1828]
 Salt Intake Reduction
Salt Intake Reduction
Studies suggest that high salt intake may have an adverse effect on asthma, particularly in men. In a small, preliminary trial, doubling salt intake for one month led to a small increase in airway reactivity (indicating a worsening of asthma) in men with asthma, as well as in non-asthmatics. [BMJ 1988;297:454] At least four double-blind trials have provided limited evidence of clinical improvement following a period of sodium restriction. It is difficult to compare the results of these studies because they used different amounts of sodium restriction. However, they consistently suggest that increased dietary sodium may aggravate asthma symptoms, especially in men. [Clin Exp Allergy 2000;30: pp.615-27]
Digestive Aids
 Hydrochloric Acid (Trial)
Hydrochloric Acid (Trial)
An older study showed that 80% of children with asthma had gastric acid secretions below normal levels.
Drug
 Corticosteroids
Corticosteroids
Inhalant forms of corticosteroid drugs will reduce the frequency and severity of asthma attacks when taken every day, but will not relieve an asthma attack once it has started. To relieve asthma symptoms, patients must use airway-opening medications (bronchodilators). When using inhalant forms of both a bronchodilator and a corticosteroid, use the bronchodilator first and then wait several minutes before using the corticosteroid.
Habits
 Tobacco Avoidance
Tobacco Avoidance
Even second-hand smoke should be avoided. In a study of passive smoke exposure, cotinine levels, when tested in asthmatic children, correlated with their bronchial sensitivity. The higher the level of cotinine in the child's urine, the worse the child's bronchial sensitivity. This held true for adults also. [Clin Chem 1999;45(4): pp.505-9]
Laboratory Testing
 Test for Food Allergies
Test for Food Allergies
Many studies have indicated that food allergies play an important role in asthma. Negative reactions to food may be immediate or delayed. Immediate onset sensitivities in children are usually due to egg, fish, shellfish, nuts, or peanuts. Foods most commonly associated with delayed onset include milk, chocolate, wheat, citrus, and food colorings. Elimination diets have been successful in treating asthma, especially for infants.
Mineral
 Magnesium
Magnesium
Magnesium levels are frequently low in asthmatics [J Lab Clin Med 1940;26: pp.340-4]. Current evidence suggests that high dietary magnesium intake may be associated with better lung function and reduced bronchial reactivity. Intravenous injection of magnesium has been reported in most, but not all, double-blind trials to rapidly halt acute asthma attacks.
Magnesium supplements may reduce the bronchoconstriction in asthma by relaxing the muscle around the bronchial tubes. Intravenous solutions containing magnesium and other nutrients have been used successfully to break acute asthma attacks. Oral use improves breathing in asthmatics and the improvement correlates with serum magnesium levels.
In a preliminary trial, 18 adults with asthma took 300mg of magnesium per day for 30 days and experienced decreased bronchial reactivity. [Magnesium-Bulletin 1997;19: pp.4-6] However, a double-blind trial investigated the effects of 400mg per day for three weeks and found a significant improvement in symptoms, but not in objective measures of airflow or airway reactivity. [Eur Respir J 1997;10: pp.2225-9] The amount of magnesium used in these trials was 300-400mg per day (children take proportionately less based on their body weight).
 Molybdenum
Molybdenum
Molybdenum may be useful in the treatment of certain cardiovascular conditions, asthma, allergies and mercury toxicity. Because of its involvement with sulfur, it may be warranted to use in asthma that is associated with sulfite sensitivity.
 Selenium
Selenium
People with low levels of selenium have a high risk of asthma. [Clin Sci 1989;77: pp.495-500] Asthma involves free-radical damage [N Engl J Med 1991;325: pp.586-7 (letter)] that selenium might protect against. In a small double-blind trial, supplementation with 100mcg of sodium selenite (a form of selenium) per day for 14 weeks resulted in clinical improvement in six of eleven patients, compared with only one of ten in the placebo group. [Allergy 1993;48: pp.30-6] Most doctors recommend 200mcg per day for adults (and proportionately less for children) – a higher, though still safe, level.
Oxygen/Oxidative Therapies
Physical Medicine
 Calming / Stretching Exercises
Calming / Stretching Exercises
Studies conducted at yoga institutions in India have reported impressive success in improving asthma. For example, one study of 255 asthma patients found that yoga resulted in improvement or cure in 74% of cases. Another study of 114 patients treated over one year by yoga found a 76% rate of improvement or cure and that asthma attacks could usually be prevented by yoga methods without resorting to drugs.
Another Indian study of 15 people with asthma claimed a 93% improvement rate over a 9-year period. That study found improvement was linked with improved concentration, and the addition of a meditative procedure made the treatment more effective than simple postures and breathing exercises. Yoga practice also resulted in greater reduction in anxiety scores than drug therapy. Its authors believe that yoga practice helps patients through enabling them to gain access to their own internal experience and increased self-awareness.
A study of 46 adolescents with asthma found that yoga practice resulted in a significant increase in pulmonary function and exercise capacity and led to fewer symptoms and medications. Patients were given daily training in yoga for 90 minutes in the morning and one hour in the evening for 40 days. Practice included yogic cleansing procedures (kriyas), maintenance of yogic body postures (asanas), and yogic breathing practices (pranayama).
Supplements
 Lycopene
Lycopene
Lycopene helps reduce the symptoms of asthma caused by exercising. In one double-blind trial [Allergy 2000;55: pp.1184-9], over half of people with exercise-induced asthma had significantly fewer asthma symptoms after taking capsules containing 30mg of lycopene per day for one week compared to when they took a placebo.
Vitamins
 Bioflavonoids
Bioflavonoids
Quercetin appears to be important in the prevention of asthma attacks. It has been shown to inhibit histamine release from mast cells and basophils when stimulated by antigens (triggers). In addition, quercetin has both a vitamin C-sparing effect and a direct stabilizing effect on membranes, including mast cells. It is also an antioxidant. Other flavones also inhibit histamine release, but to a lesser degree.
 Vitamin C (Ascorbic Acid)
Vitamin C (Ascorbic Acid)
Supplementation with 1gm of vitamin C per day reduces the tendency of the bronchial passages to go into spasm [Lung 1976;154: pp.17-24], an action that has been confirmed in double-blind research. [Ann Allergy 1990;65: pp.311-4] This amount of vitamin C, while providing benefit, is not curative. Beneficial effects of short-term vitamin C supplementation (i.e., less than three days) have been observed. In one double-blind trial, 500mg of vitamin C per day for two days prevented attacks of exercise-induced asthma. [Ann Allergy 1982;49: pp.146-51]
Both treated and untreated asthmatic patients have been shown to have significantly lower levels of ascorbic acid in both serum and white blood cells. Ascorbic acid has a wide variety of pharmacological effects that appear important in asthmatic treatment.
 Vitamin B12 (Cobalamine)
Vitamin B12 (Cobalamine)
In one clinical trial, weekly 1,000mcg intramuscular injections produced definite improvement in asthmatic children. Of 20 patients, 18 showed less shortness of breath on exertion, as well as improved appetite, sleep, and general condition. When given sublingually prior to a sulfite challenge, vitamin B12 appears to be especially effective in cases of asthma caused by sulfite sensitivity.
 Folic Acid
Folic Acid
A research team at Johns Hopkins found that individuals with the lowest blood levels of folic acid are at a significantly increased risk of skin and respiratory allergies, wheezing, and asthma.
 Vitamin B6 (Pyridoxine)
Vitamin B6 (Pyridoxine)
Vitamin B6 deficiency is common in asthmatics. [Ann Allergy 1975;35: pp.153-8] This deficiency may relate to the asthma itself or to certain asthma drugs (such as theophylline and aminophylline) that deplete vitamin B6. [Ann Allergy 1990;65: pp.59-62] In a double-blind trial, 200mg per day of vitamin B6 for two months reduced the severity of asthma in children and reduced the amount of asthma medication they needed. [Ann Allergy 1975;35: pp.93-7] In another trial, asthmatic adults experienced a dramatic decrease in the frequency and severity of asthma attacks while taking 50mg of vitamin B6 twice per day. [Am J Clin Nutr 1985;41: pp.684-8] Nonetheless, the research remains somewhat inconsistent, and one double-blind trial found that high amounts of B6 supplements did not help asthmatics who required the use of steroid drugs. [Ann Allergy 1993;70: pp.141-52]
Click to see sample report
Your body is a highly complex, interconnected system. Instead of guessing at what might be wrong, let us help you discover what is really going on inside your body based on the many clues it is giving.
Our multiple symptom checker provides in-depth health analysis by The Analyst™ with full explanations, recommendations and (optionally) doctors available for case review and answering your specific questions.
KEY













