Rheumatoid Arthritis: Overview
Arthritis is any disorder that affects joints. Rheumatoid Arthritis (RA) is an inflammatory disease that causes pain, swelling, stiffness, and loss of function in the joints. It has several features that distinguish it from other kinds of arthritis.
- see your health summarized and in detail
- let The Analyst™ find what's wrong
- learn what you should be doing right now
A movable joint is a place where the ends of two bones meet and move relative to each other. Movable joints are surrounded by a joint capsule enclosed in a synovial membrane (the synovium) that produces and contains synovial fluid.
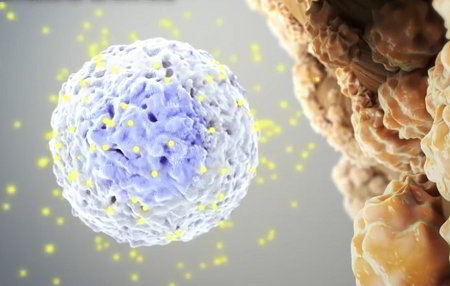
This clear fluid protects, lubricates, supports, and nourishes the cartilage and bones inside the joint capsule. Cartilage covers and cushions the ends of the two bones.
In Rheumatoid Arthritis, the immune system for reasons unknown attacks a person's own cells inside the joint capsule. White blood cells that are part of the normal immune system travel to the synovium and release cytokines that attack synovial cells, which in turn release other destructive substances.
These destructive substances cause the synovial membrane to grow new blood vessels and form a thickened area called a pannus. As the pannus grows it invades and destroys areas of bone and cartilage.
This destruction leads to an inflammatory process (synovitis) in which the cells of the synovium grow and divide abnormally, making the normally thin synovium thick. Fluid builds up inside the joint, resulting in a joint that is swollen, puffy to the touch, warm, red, and painful – the classic symptoms of RA.
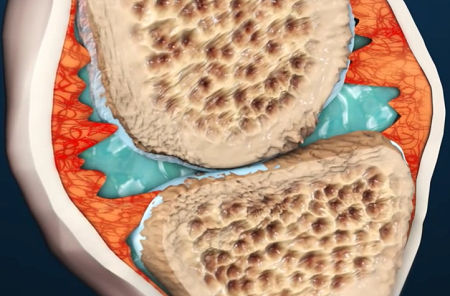
As RA progresses and continues to destroy cartilage and bone within the joint, the surrounding muscles, ligaments, and tendons that support and stabilize the joint become weak and unable to work normally. All of these effects lead to the pain and deformities often seen in RA.
This process can eventually lead to ankylosis, in which the bones grow together (fuse) and become immobile, making it impossible to move the joint.
Doctors studying RA now believe that damage to bones begins during the first year or two that a person has the disease and this is one reason early diagnosis and treatment are so important.
Incidence; Causes and Development; Contributing Risk Factors
Rheumatoid Arthritis is the second-most common type of arthritis and affects some 0.7% of Americans, three times more women than men. Onset is usually in middle-age, but also occurs in the 20s and 30s.
Bacterial
Researchers suspect that some type of microorganism may be the trigger in some people who have an inherited tendency for the disease. Dr. Hoekstra, MD has found that virtually all the patients he has studied have had significant amounts of a bacteria called Propionibacterium acnes. "This is the genus and species of the organism we believe is responsible for propagating and perpetuating this disease," says Dr. Hoekstra. "It is a very common bacteria in an altered state of being – it is cell wall deficient."
The bacterium was first identified and described in 1981 by G.A. Denys at Wayne State University in Detroit, Michigan. "This bacteria is passed transplacentally, from mother to fetus, and this may be responsible for RA showing up in generations in a single family," says Dr. Hoekstra. Why this bacteria is prevalent in seemingly all cases of RA is not clear, but overuse of antibiotics may be a factor encouraging its growth. "The use of antibiotics is one of the most potent ways of inducing cell wall deficiency; bacteria seem to do this as a survival mechanism." In other words, when a bacterium is transformed into a cell wall deficient form, it assumes different characteristics from the whole or native type of microorganism it used to be.
Dr. Hoekstra explains, "The organism remains intact except for losing its cell wall and its antigenic characteristics, enabling it to function as a cellular chameleon." When it loses its antigenic signature, the bacteria are able to mask themselves against destruction by the immune system's antibodies which can no longer recognize them as antigens (foreign proteins).
Dr. Hoekstra's mentor, Lida Holmes Mattman, Ph.D., also of Wayne State confirmed the causal role of P. acnes in a laboratory experiment. Dr. Mattman extracted the bacteria from the synovial fluid (which lubricates joints) of human arthritis patients, and injected it into chicken embryos. The chicks then exhibited symptoms of RA. When she treated the chicks with antibiotics known to disable P. acnes, the disease disappeared.
Exhausted Immune System
Another recently discovered aspect of RA is that sufferers who were previously thought to have overactive immune systems, instead may have exhausted immune systems. ''What this study has shown for the first time is that patients with RA have prematurely aged immune systems'' said lead author Dr. Cornelia Weyand, a rheumatologist at the Mayo Clinic.
''Until now we have thought that these patients had overactive immune systems, which is why we have aggressively treated the symptoms of rheumatoid arthritis with medications that suppress the immune system." Weyand and colleagues studied the immune systems of 51 patients with rheumatoid arthritis and compared them to 47 people of similar age who did not have the condition. They found that the T-cells – the immune cells that are programmed to recognize and attack invaders such as bacteria and viruses – were worn out. ''They do not make new T-cells.'' [Proceedings of the National Academy of Sciences, 2000]
Tea and decaffeinated coffee intake were individually associated with an increased risk of developing rheumatoid arthritis in a prospective study of 64,000 black women followed for up to 4 years. Caffeinated coffee intake was not associated with the risk of developing RA. [65th Annual Scientific Meeting of the American College of Rheumatology and the 36th Annual Scientific Meeting of the Association of Rheumatology Health Professionals, November 11-15, 2001, San Francisco, CA; presentation 1938]
Signs and Symptoms
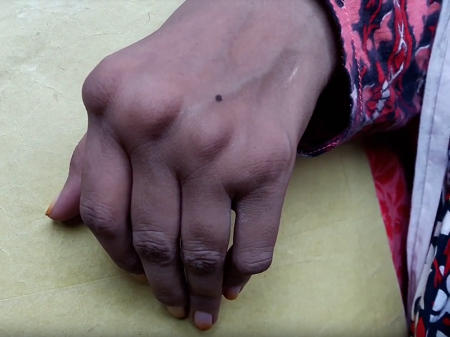
Rheumatoid Arthritis generally occurs in a symmetrical pattern so that if one knee or hand is involved, the other one is also. The disease almost always affects the wrists and hands (especially the finger joints closest to the hand) but can also affect the knees, neck, shoulders, elbows, ankles, feet, hips, and even the jaw and spine.
Some people also experience the effects of RA in places other than the joints; about one-quarter develop rheumatoid nodules – bumps under the skin – that often form close to the joints. It can affect the eyes, skin, heart, lungs, kidneys, nervous system, and digestive tract.
The signs and symptoms of RA include:
- Pain and stiffness lasting for more than 30 minutes in the morning or after a long rest.
- Tender, warm, swollen joints. Joint inflammation often affecting the wrist and finger joints closest to the hand; other affected joints can include those of the neck, shoulders, elbows, hips, knees, ankles, and feet. Rheumatoid nodules are sometimes present.
- Symmetrical pattern. For example, if one knee is affected, the other one is also.
- Fatigue, occasional fever, a general sense of not feeling well (malaise).
- Symptoms possibly lasting for many years.
- Symptoms affecting other parts of the body besides the joints.
Diagnosis and Tests
RA can be difficult to diagnose in its early stages for several reasons. First, there is no single test for the disease. In addition, symptoms differ from person to person and can be more severe in some people than in others. Furthermore, symptoms can be similar to those of other types of arthritis and joint conditions, and it may take some time for other conditions to be ruled out as possible diagnoses. Finally, the full range of symptoms develops over time, and only a few symptoms may be present in the early stages.
Doctors use a variety of tools to diagnose the disease and to rule out other conditions: medical history, physical examination, laboratory tests. One common test is for rheumatoid factor, an antibody that is eventually present in the blood of most RA patients. Not all people with RA test positive for rheumatoid factor, especially early in the disease; indeed some who do test positive never develop the disease.
Other common tests include some that indicate the degree or severity of inflammation in the body (the erythrocyte sedimentation rate, or C-reactive protein), a white blood cell count, and a blood test for anemia. X-rays can be used to determine the degree of joint destruction but are not useful in the early stages of RA before bone damage is evident. They can be used later to monitor the progression of the disease.
Treatment and Prevention
There is currently no cure for Rheumatoid Arthritis. Although RA can have serious effects on a person's life and well-being, current treatment strategies – including pain relief and other medications, a balance between rest and exercise, and patient education and support programs – allow most people with the disease to lead active and productive lives. In recent years, research has led to a new understanding of RA and has increased the likelihood that, in time, researchers can find ways to greatly reduce the impact of this disease.
When other treatments don't work, surgical joint replacement (arthroplasty) or joint fusion (arthrodesis) are options for both large and small joints.
Prognosis; Complications
RA varies a lot from person to person. For some it lasts only a few months to a year or two and goes away without causing any noticeable damage. Others have mild or moderate disease, with periods of worsening symptoms, called flares, and periods in which they feel better, called remissions. Still others have severe disease that is active most of the time, lasts for many years, and leads to serious joint damage and disability.
Many people with RA develop anemia, or a decrease in the normal number of red blood cells. Other effects, which occur less often, include neck pain and dry eyes and mouth. Very rarely, people may have inflammation of the blood vessels, the lining of the lungs, or the sac enclosing the heart.
People with Rheumatoid Arthritis are more prone to atherosclerosis, and risk of myocardial infarction (heart attack) and stroke is markedly increased.
Signs, symptoms & indicators of Rheumatoid Arthritis:
Lab Values - Cells
 Low lymphocyte count
Low lymphocyte count
Autoimmune problems such as rheumatoid arthritis can cause reduced lymphocyte counts.
Lab Values - Chemistries
Symptoms - Environment
 (Minor/major) pain in cold/cool/damp weather
(Minor/major) pain in cold/cool/damp weather
Cold, damp weather is well known for aggravating aching bones. Rheumatoid arthritis can flare up during winter months; what might be a dull ache during the summer can become a shooting pain during the winter.
 No pain in cold/cool/damp weather
No pain in cold/cool/damp weather
Cold, damp weather is well known for aggravating aching bones. Rheumatoid arthritis can flare up during winter months; what might be a dull ache during the summer can become a shooting pain during the winter.
Symptoms - General
Symptoms - Head - Eyes/Ocular
 (Very) dry eyes
(Very) dry eyes
"Dry eye" is a symptom of certain autoimmune diseases like rheumatoid arthritis and Sjogren's syndrome.
 (Very) watery eyes
(Very) watery eyes
"Dry eye" is a symptom of certain autoimmune diseases like rheumatoid arthritis and Sjogren's syndrome.
Symptoms - Metabolic
Symptoms - Nails
Symptoms - Skeletal
 Variable duration morning stiffness or morning stiffness for 45-120 minutes or morning stiffness lasting hours
Variable duration morning stiffness or morning stiffness for 45-120 minutes or morning stiffness lasting hours
Rheumatoid arthritis patients often complain of prolonged morning stiffness or pain which may last 45 minutes or longer.
 Heberden's nodes
Heberden's nodes
Rheumatoid arthritis sufferers also experience swelling/bumps in the same joints that are affected by Heberden's nodes, but the bumps are not the same.
 Morning stiffness that eases rapidly
Morning stiffness that eases rapidly
Rheumatoid arthritis patients often complain of prolonged morning stiffness or pain which may last 45 minutes or longer.
Conditions that suggest Rheumatoid Arthritis:
Aging
 Hearing Loss
Hearing Loss
Rarely, rheumatoid arthritis affects the joints between the ossicles and can cause conductive hearing loss.
Autoimmune
 Gluten Sensitivity / Celiac Disease
Gluten Sensitivity / Celiac Disease
People with Rheumatoid Arthritis have a higher risk of also being diagnosed with Celiac Disease.
Dental / Oral
Immunity
 Chronic Fatigue / Fibromyalgia Syndrome
Chronic Fatigue / Fibromyalgia Syndrome
Almost all (98%) of Rheumatoid Arthritis patients report fatigue. They also report that it is more of a problem than the stiffness and pain.
Lab Values
Musculo-Skeletal
Nutrients
 Zinc Requirement
Zinc Requirement
There is a possibility that zinc malabsorption may contribute to low zinc levels amongst rheumatoid arthritics. [J Rheumatol. 1997;24(4): pp.643-6] While levels of zinc have been found to be lower than normal in the blood of patients with rheumatoid arthritis, supplementation does not appear to be beneficial to the condition.
Sleep
Symptoms - Skeletal
Risk factors for Rheumatoid Arthritis:
Diet
Digestion
 Ulcerative Colitis
Ulcerative Colitis
Joint inflammation can occur from the overactive immune system seen in ulcerative colitis. This problem may go away when the colitis is treated.
Glandular
Rheumatoid Arthritis suggests the following may be present:
Autoimmune
 Chronic Thyroiditis
Chronic Thyroiditis
A study of 91 patients with rheumatoid arthritis found 29 patients had evidence of thyroid dysfunction compared to 10 of the 93 controls. The excess thyroid dysfunction was due to either hypothyroidism or Hashimoto's thyroiditis. In this study, thyroid dysfunction is seen at least 3 times more often in women with rheumatoid arthritis than in women with similar demographic features with non-inflammatory rheumatoid diseases such as osteoarthritis and fibromyalgia. [Annals of Rheumatic Diseases, 1993;52 pp.454-456]
Digestion
 Atrophic Gastritis
Atrophic Gastritis
Chronic atrophic gastritis occurs in up to 63% of rheumatoid arthritis patients. Achlorhydria also occurs frequently and is associated with changes in gastric microbial patterns.
 Hydrochloric Acid Deficiency
Hydrochloric Acid Deficiency
Lack of stomach acid occurs frequently in rheumatoid arthritis patients. This is associated with changes in gastric microbial patterns.
 Bacterial Dysbiosis
Bacterial Dysbiosis
Immunologic responses to gut flora have been advanced by several authors as being important causative factors of inflammatory joint diseases. It is well-known that reactive arthritis can be activated by intestinal infections with Yersinia, Salmonella and other enterobacteria. In some cases bacterial antigens have been found in synovial cells and may enter the circulation because of the increased intestinal permeability associated with the intestinal infection. Increased intestinal permeability and immune responses to bacterial debris may cause other types of inflammatory joint disease as well.
Glandular
 Hypothyroidism
Hypothyroidism
A study of rheumatoid arthritis patients found evidence of thyroid dysfunction 3 times more often than in controls. The excess thyroid dysfunction was due to either hypothyroidism or Hashimoto's thyroiditis. [Annals of Rheumatic Diseases, 1993;52 pp.454-6]
Hormones
 Low DHEA Level
Low DHEA Level
DHEA levels have been found to be low in women with rheumatoid arthritis, a condition frequently associated with osteoporosis. In a study of 49 postmenopausal women with rheumatoid arthritis, DHEA levels (measured as DHEA-S) were significantly lower than in healthy controls. [Gaby, AR. Holistic Medicine. Spring, 1993: p.22]
Immunity
 Weakened Immune System
Weakened Immune System
People with rheumatoid arthritis, who for a long time were thought to have overactive immune systems, instead may have exhausted immune systems. A study at the Mayo Clinic has shown for the first time that patients with rheumatoid arthritis have prematurely aged immune systems. Patients 20 to 30 years old had a collection of T-cells that looked like they belonged to 50 to 60 year olds.
 Immune System Imbalance (TH2 Dominance)
Immune System Imbalance (TH2 Dominance)
A Mayo Clinic study found that the T-cells were 'worn out' in rheumatoid arthritis patients, who do not make new T-cells as readily as they should.
Mental
 Depression
Depression
Studies report that around 30% of people suffering from inflammatory diseases such as rheumatoid arthritis are depressed – more than four times higher than the general population.
Musculo-Skeletal
 Osteoporosis - Osteopenia
Osteoporosis - Osteopenia
According to researchers, women with rheumatoid arthritis have up to double the risk of developing osteoporosis and those who use steroid drugs to help control the arthritis are at an even higher risk of bone loss. [Arthritis and Rheumatism, March 2000]
Nutrients
 EFA (Essential Fatty Acid) Type 3 Requirement
EFA (Essential Fatty Acid) Type 3 Requirement
Aching, swollen joints may just be demanding the right kind of oil. Shifting the body's balance toward omega-3 oils and away from omega-6 oils significantly alleviates symptoms in patients with rheumatoid arthritis, according to a recent study in the Journal of Rheumatology.
Rheumatoid Arthritis can lead to:
Dental / Oral
 Periodontal Disease - Gingivitis
Periodontal Disease - Gingivitis
People with Rheumatoid Arthritis (RA) are 8 times more likely to have gum disease. In addition, those with RA can have trouble brushing and flossing due to finger joint damage.
Digestion
Musculo-Skeletal
 TMJ Problems
TMJ Problems
If the TMJ is affected by rheumatoid arthritis, it is usually one of the last joints involved. RA affects the TMJ in almost 20% of cases. Pain, swelling, and limited movement are the most common symptoms.
Rheumatoid Arthritis could instead be:
Infections
 Lyme Disease
Lyme Disease
The symptoms of Lyme disease have frequently been misdiagnosed as rheumatoid arthritis and subsequently mistreated.
Recommendations for Rheumatoid Arthritis:
Amino Acid / Protein
 Thymic Factors
Thymic Factors
The thymus gland contributes to the maturing of T-cells. Thymus gland extracts will assist this process when the thymus gland is shrunken, as happens commonly in aging. Through his clinical experiences with thymic supplementation, Dr. Burgstiner said he observed 28 cases of rheumatoid arthritis cases go into remission where patients no longer needed to use prednisone, methotrexate or gold shots.
 L-Phenylalanine
L-Phenylalanine
The 'D' form of phenylalanine (DPA) has been used to treat chronic pain, including rheumatoid arthritis, with mixed effectiveness.
Botanical / Herbal
 Turmeric Extract, Curcumin
Turmeric Extract, Curcumin
Clinical studies have substantiated curcumin anti-inflammatory effects, including a significant beneficial effect in Rheumatoid Arthritis. In one study, curcumin was compared to phenylbutazone, a very potent NSAID that has fallen out of favor because of frequent side effects. The improvements in the duration of morning stiffness, walking time, and joint swelling were comparable in both groups.
 Cat's Claw
Cat's Claw
Uncaria tomentosa extract over a 6-month period reduced the number of painful joints in a well-controlled study involving 40 patients with active rheumatoid arthritis already being treated with sulfasalazine or hydroxychloroquine. An additional 7 months of treatment with Uncaria tomentosa extract reduced the number of painful and swollen joints with the same group of patients. [J Rheumatol 2002;29(4): pp.678-81]
 Boswellia
Boswellia
Boswellin is the first herbal remedy to have documented clinical evidence that it is useful in rheumatoid arthritis, osteoarthritis, low back pain, soft tissue rheumatism and myositis symptoms.
 Picrorhiza
Picrorhiza
Open-label studies conducted in India show a preliminary benefit for persons with primarily rheumatoid arthritis. [Langer JG, Gupta OP, Atal CK (1981) "Clinical trials on Picrorhiza kurroa" Ind J Pharmacol 13: pp.98-103 (review)] More study is needed before any definite conclusions can be drawn.
See also [T Hart BA, Simons JM, Knaan-Shanzer S, et al. Antiarthritic activity of the newly developed neutrophil oxidative burst antagonist apocynin. Free Rad Biol Med 1990;9: pp.127-31]
Chinese Medicine
 Lei Gong Teng
Lei Gong Teng
Treatment with an extract of Tripterygium wilfordii Hook F (360-570mg per day) improved clinical manifestations and laboratory findings in a study of 13 patients with rheumatoid arthritis. Three patients withdrew during the first 16 weeks of dose escalation, including one patient who developed diastolic hypertension at a dose of 180mg per day. [J Rheumatol 2001;28(10): pp.2160-7]
Diet
 Plant-Based Nutrition
Plant-Based Nutrition
Many studies have shown that vegetarian diets can be used to successfully treat rheumatoid arthritis.
Researchers in one study found that participants who ate the greatest number of servings of cooked vegetables were about 75% less likely to develop rheumatoid arthritis than those who reported eating the fewest servings. [American Journal of Clinical Nutrition: November 1999;70: pp.1077-82]
"... 43 patients with rheumatoid arthritis, those assigned to a vegan diet... had improvement in rheumatoid arthritis symptoms." [British J Rheumatology, 36(1) 1997]
 Monounsaturated Oils
Monounsaturated Oils
Researchers found that people who used the most olive oil were significantly less likely to develop rheumatoid arthritis than people who consumed the least. [American Journal of Clinical Nutrition: November 1999;70: pp.1077-82]
 Dairy Products Avoidance
Dairy Products Avoidance
For some people, the type of protein contained in dairy products appears to contribute to arthritis pain by irritating the tissue around their joints. Many of them find relief by switching to a vegan diet – which contains no animal products whatsoever.
Here is a letter received by Robert Cohen, arch enemy of the dairy industry and despised by most dairy farmers. The letter was sent to him in January, 2002 by a long-time dairy farmer and speaks for itself:
You and I have stood on different sides of the fence for a number of years, but I've got a story to tell you, and an apology to offer. Catherine (my wife of 21 years) and I both grew up on dairy farms. We've been raising Holsteins as long as we can remember. Cath is just 42 years old, but she is crippled with rheumatoid arthritis. There is no record of this disease in her family, but she has been in pain for the past two years, much of it bedridden.
We've tried traditional and alternative therapies and medicines, but she only got a little short term relief. We even tried acupuncture. Try finding an acupuncturist in the rural Midwest! It was expensive, and didn't really work. Catherine's pain has been unbearable at times.
Despite there being no information on the internet linking dairy consumption to rheumatoid arthritis, and nothing in medical journals (I've searched online Medline), we made a resolution together to discontinue drinking our own milk, and not eat cheese or any other dairy product for six months, just to see if there would be some improvement.
I have to tell you this. Catherine feels like she's been to Lourdes. She's cured. There is some pain, but most is gone. I've had changes too which I'll discuss some other time. I thank you, and curse you at the same time. Milking cows is my livelihood. I've always believed that what I was doing was the right thing. I'm not going to sell my cows and sell my farm. I love the business. I just don't feel that good about it anymore. You were right about the arthritis. I don't know about the cancer and heart attacks, but you have given us a miracle that doctors were not able to provide. It did not take us three to six months to learn the truth. It took just three weeks. I've ridiculed your work in the past. Please accept my apology.
Your friend,
Tom
Since this type of joint pain can be a symptom of food allergy, dietary change may have a profound effect. Dairy products – the most common food allergen – are one likely causative factor.
"In the case of the eight year old female subject, juvenile rheumatoid arthritis was a milk allergy. After avoiding dairy products, all pain was gone in three weeks." [Journal of the Royal Society of Medicine, 1985, 78]
"In systemic arthritis, like Rheumatoid, the cause is coursing through the blood, and it got there through the diet. When all of the joints are involved, the cause is not physical, but chemical. It's usually casein. (80% of milk protein is casein)." ["No Milk", by Daniel Twogood, D.C.]
"Certain foods trigger the symptoms of rheumatoid arthritis, and eliminating these foods sometimes causes even long-standing symptoms to improve or even remit entirely. It is important to avoid the problem foods completely, as even a small amount can cause symptoms. All dairy products should be avoided: skim or whole cow's milk, goat's milk, cheese, yogurt, cream, etc." [Neal Barnard, M.D. Physicians Committee for Responsible Medicine]
 Therapeutic Fasting
Therapeutic Fasting
The fast allows the entire system to restore its cellular and immunogenic integrity. Fasting can cause regression of some autoimmune and inflammatory disorders, such as rheumatoid arthritis. [Controlled trial of fasting and a one-year vegetarian diet eased symptoms of rheumatoid arthritis; The Lancet, 1991, 338]
 Nightshade Family Food Avoidance
Nightshade Family Food Avoidance
Elimination of nightshade family foods does not help all people with arthritis, but people who respond are usually helped a great deal.
Drug
Hormone
 DHEA
DHEA
The incidence of osteoporosis is elevated in women with rheumatoid arthritis. DHEA levels correlated significantly with, and were predictive of, bone mineral density, even after corticosteroid therapy was taken into account. Raising DHEA levels by supplementation in these women should reduce the risk of osteoporosis. [Gaby, AR. Holistic Medicine. Spring, 1993: p.22]
Dr. Hackethal has observed some rheumatoid patients taking DHEA become well even when C-reactive protein and Rh- factor are positive.
Laboratory Testing
 Test for Food Allergies
Test for Food Allergies
While virtually any food can result in aggravation of rheumatoid arthritis, the most common offending foods are dairy protein, wheat, corn, citrus fruits, eggs, beef, sugar, fats, salt, caffeine and nightshade (Solanum) family foods (tomato, potato, eggplants, peppers and tobacco).
In order to test whether foods trigger symptoms, a food elimination protocol was followed in a blind, placebo-controlled study that resulted in significant improvement in arthritic symptoms, including shorter duration of morning stiffness and fewer painful joints. [Lancet 1986:1, pp.236-8]
While many doctors believe that the percentage of rheumatoid arthritis patients benefiting from diet manipulation is small, there is an increasing number of scientific studies suggesting that food elimination may help a higher percentage of patients.
"Nutritional therapy, not drugs, is the cornerstone of alternative treatment. A treatment for arthritis that relieves symptoms in a large percentage of patients is based on the theory that most arthritic symptoms are allergic reactions." [Jane Heimlich (wife of Dr. Henry Heimlich, the "Heimlich Maneuver" physician), in her book, "What Your Doctor Won't Tell You"]
 Test Zinc Levels
Test Zinc Levels
Zinc levels amongst patients with rheumatoid arthritis are usually reduced. Results from zinc supplementation trials amongst rheumatoid arthritis patients have been mixed, though most find some improvement.
 Bacteria / Pathogen Testing by PCR
Bacteria / Pathogen Testing by PCR
An Autoimmune/Arthritis Disease Panel (Blood) can test for the presence of Mycoplasma fermentans, Mycoplasma pneumoniae and Epstein Barr Virus (EBV).
Mineral
 Manganese
Manganese
Manganese functions in the antioxidant enzyme superoxide dismutase (manganese SOD), which is deficient in patients with rheumatoid arthritis. Manganese supplementation has been shown to increase SOD activity, indicating increased antioxidant activity. A good dosage for a manganese supplementation is 5 to 15mg per day.
 Selenium
Selenium
Selenium levels are generally low in patients with rheumatoid arthritis. Low selenium levels in joint tissues may be a significant factor contributing to the inflammatory process in rheumatoid arthritis. Selenium plays an important role as an antioxidant and serves as the mineral cofactor in the free-radical scavenging enzyme glutathione peroxidase. This enzyme is also important in reducing the production of inflammatory compounds that cause much of the damage to tissues seen in rheumatoid arthritis. A deficiency of selenium would result in even more significant damage.
 Boron
Boron
There is increasing evidence that boron is an essential trace element for both man and animal. It does influence calcium and magnesium metabolism, and this is possibly through the parathyroid gland. It does alleviate and seems to cure arthritis either by acting against whatever organism may cause rheumatoid diseases and/or as a membrane catalyst that permits repair of damaged cartilage and collagen.
 Copper
Copper
Copper has a mild anti-inflammatory effect. The use of copper bracelets in the treatment of arthritis has a long history, and wearers continue to claim positive results. The copper in the bracelets reacts with the fatty acids in the skin to form copper salts that are absorbed into the body. The copper salts may cause a blue-green stain on the skin, but this can be removed with soap and water. Recent research suggests that copper salicylate used to treat arthritis reduces symptoms more effectively than either copper or aspirin alone.
 MSM (Methyl Sulfonyl Methane)
MSM (Methyl Sulfonyl Methane)
The reason why MSM is beneficial against arthritis is unclear. It may be because of its sulfur content, or because of its anti-inflammatory and analgesic properties. Unlike aspirin, which offers immediate pain relief, MSM takes 3 to 4 weeks before it produces noticeable change, except in rheumatoid patients who have been known to feel differences in just one day, and almost always within 3 to 4 days.
In an animal study on rheumatoid arthritis-like joint degeneration, MSM was effective in reducing joint inflammation, and completely prevented the breakdown of cartilage. According to Dr. Stanley Jacobs, MD, MSM can be helpful in most musculoskeletal pain and inflammation, including rheumatoid arthritis.
Oxygen/Oxidative Therapies
 Ozone / Oxidative Therapy
Ozone / Oxidative Therapy
Many people with arthritis report that the hydrogen peroxide bath has helped them greatly.
Physical Medicine
 Calming / Stretching Exercises
Calming / Stretching Exercises
According to a 1994 study published in the British Journal of Rheumatology, 20 patients with rheumatoid arthritis participated in a yoga program. Left hand grip strength improved significantly and all patients who completed the course expressed the desire to continue after the study.
Supplements
 Essential Fatty Acids
Essential Fatty Acids
Both Omega-6 and Omega-3 EFAs and their metabolites Gamma Linolenic Acid (GLA) and EPA have shown effectiveness against Rheumatoid Arthritis. One study showed that use for 12 months produced meaningful improvement in 76% of subjects. The oil from cold water fish falls into the Omega-3 category, and has shown positive results in reducing inflammation. Some researchers believe that if you regularly eat small amounts of cold-water fish over many years, you may be able to avoid rheumatoid arthritis.
 Superoxide Dismutase
Superoxide Dismutase
In a Danish study, arthritis patients were treated with injections of superoxide dismutase, an enzyme containing copper (or manganese and zinc) that is found within the cells. Many obtained relief from symptoms such as joint swelling, pain and morning stiffness.
Vitamins
 Vitamin B6 (Pyridoxine)
Vitamin B6 (Pyridoxine)
When nodules (Heberden's nodes) are present, vitamin B6 at 100-150mg per day may help. One doctor reports seeing even better results if one handful of raw pecans is eaten every day. The nodes may not go away but pain and mobility are better over several weeks.
 Vitamin B5 (Pantothenic Acid)
Vitamin B5 (Pantothenic Acid)
Low pantothenic acid levels are implicated in the development of human osteoarthritis and rheumatoid arthritis, as whole blood pantothenic acid levels have been reported to be lower in rheumatoid arthritis patients compared with normal controls. In addition, disease activity was inversely correlated with pantothenic acid levels.
Click to see sample report
Your body is a highly complex, interconnected system. Instead of guessing at what might be wrong, let us help you discover what is really going on inside your body based on the many clues it is giving.
Our multiple symptom checker provides in-depth health analysis by The Analyst™ with full explanations, recommendations and (optionally) doctors available for case review and answering your specific questions.
KEY













