Allergic Rhinitis / Hay Fever: Overview
Alternative names: Hay fever (Note that despite its name, it is not caused by hay, and does not produce a fever.)
Allergic rhinitis is inflammation of the inside the nose that occurs when the immune system reacts to allergens in the air as if they were harmful.
- understand what's happening to your body
- let The Analyst™ find what's wrong
- check your overall health status
Incidence; Causes and Development; Contributing Risk Factors
Allergic rhinitis is the most common form of allergy, estimated to affect roughly 1-in-5 people.

It is caused by the body's immune system overreacting to irritants in the environment and producing antibodies to fight them off. Common examples of irritants are:
- Pollens, grasses, or ragweed (in certain seasons and areas), causing 'hay fever'
- Dust, chemicals found in house dust mite excrement, cockroaches
- Animal dander (flakes of skin)
- Droplets of urine or saliva from certain animals
- Mold and fungus spores
- Spicy foods
During an allergic episode, the immune system releases chemicals that cause the mucous membrane inside the nose to become swollen, and excess mucus to be produced.
The following may increase the risk of having allergic reactions:
- A family history of allergies
- Asthma
- Atopic syndrome (a tendency to be hyperallergic)
- Smoking or prolonged exposure to second-hand smoke
- Wood smoke and other air pollution
- Airborne fumes and chemicals such as hairspray, perfumes
- Changes in temperature or humidity, wind
Signs and Symptoms
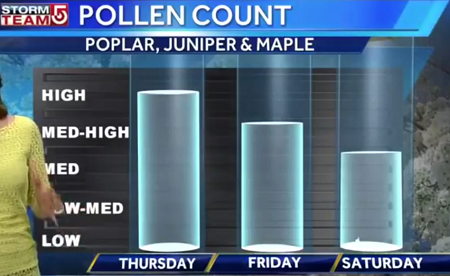
For many people, symptoms vary with the seasons, which is why the term 'pollen season' exists and weather reports often include a 'pollen forecast' and 'pollen count'. For others, it is a year-round problem.
Symptoms start soon after exposure to an allergen. They are usually mild, but for some people they can be severe and long-lasting, leading to sleep problems and difficulty performing everyday activities. These include:
- Blocked, stuffy or runny nose
- Sneezing
- Itchy nose and/or eyes
- Watery eyes
- Dark circles under eyes
- A sore/scratchy throat
- "Sinus" symptoms – headache, feeling of pressure behind the eye, pain above the cheekbones and on the lower forehead, aching teeth
- Coughing
- Skin rashes or hives
- Diarrhea and/or frequent urination
- Recurrent headaches and/or fatigue (generally after long-term exposure to allergens)
Diagnosis and Tests
A health care provider will examine the patient's nose and nasal secretions, and ask if they have noticed any specific allergy triggers. If the cause of allergies is not obvious, the patient may be referred to an allergist – a physician who can pinpoint the triggers by performing skin or blood tests.
Treatment and Prevention

The best way to prevent allergic rhinitis is to avoid the allergen(s) that cause it. It is often difficult to completely avoid allergens, but reducing exposure is an important step. Depending on which allergens are causing problems, a combination of the following is often effective:
- Cover pillows and mattresses with plastic covers
- Use synthetic materials (acrylic) instead of animal products (wool, feathers)
- Minimize dust-collecting household items
- Use hard floor coverings instead of carpet
- Regularly wash or vacuum fabrics and fabric-covered items such as soft toys, pillows, curtains
- Use a vacuum cleaner with a HEPA (high efficiency particulate air) filter
- Use air purifiers, dehumidifiers, or dust filters
- Clean with a damp cloth instead of dry dusting
- When the pollen count is high, stay inside, shower and change clothes after being outside, and avoid drying laundry outside
- Minimize mold and mildew exposure by keeping the house dry and well ventilated, opening windows when showering or cooking, and not storing clothes tightly packed or in damp areas
- Minimize exposure to pets by limiting them to certain rooms or (even better) keeping them outside. Wash pets every week or two, groom dogs outside, and regularly wash their bedding.
Mild allergy symptoms can be controlled by using over-the-counter long-acting, non-sedating antihistamines and by regular nasal irrigation (rinsing the nasal passages with salt water to remove irritants). Taking antihistamine medication an hour before entering a house with pets can help minimize symptoms.
If these measures are not effective, a doctor may prescribe a steroid nasal spray. Corticosteroids reduce inflammation and swelling; they take longer to work than antihistamines, but their effect lasts longer.
For more severe cases, immunotherapy – also known as hyposensitization or desensitization therapy – may be carried out under supervision. This involves repeated injections of gradually increasing amounts of the identified allergen in order to desensitize the immune system.
Allergic rhinitis may be successfully treated with alternative therapies, beginning with dietary changes. Use the tincture and homeopathic remedies for acute allergic reactions. Acupuncture, butterbur supplements, honey, and probiotics are other alternative remedies.
Complications
In some cases, allergic rhinitis can lead to nasal polyps, inability to sleep, worsening of asthma symptoms, recurring middle ear infections and/or sinus infections, reduced effectiveness at work or school, and headaches.
Signs, symptoms & indicators of Allergic Rhinitis / Hay Fever:
Lab Values - Cells
Symptoms - Allergy
Symptoms - Head - Eyes/Ocular
 (Occasional/frequent) itchy eyes
(Occasional/frequent) itchy eyes
Itching is the hallmark of allergic conjunctivitis, as well as other forms of allergic eye disease. The itching may be mild to severe. In general, a red eye in the absence of itching is not caused by ocular allergy.
Symptoms - Head - Nose
Conditions that suggest Allergic Rhinitis / Hay Fever:
Circulation
Eyes / Ocular
Metabolic
 Meniere's Disease
Meniere's Disease
Several studies have found a strong connection between inhalant allergies and Meniere's Disease.
Symptoms - Allergy
Risk factors for Allergic Rhinitis / Hay Fever:
Allergy
 Allergy to Foods (Hidden)
Allergy to Foods (Hidden)
The ear, nose, and throat are common target organs for food allergens. Congestion or inflammation of the nose (rhinitis) may be due to airborne irritants and allergens, but food allergy may be an undiagnosed cause of this common problem.
Family History
Hormones
Symptoms - Environment
 Mild/significant/severe diesel exhaust exposure
Mild/significant/severe diesel exhaust exposure
Diesel exhaust fumes and ozone can enhance the effects of inhaled allergens or have an effect on immune function.
Allergic Rhinitis / Hay Fever suggests the following may be present:
Allergy
Allergic Rhinitis / Hay Fever can lead to:
Dental / Oral
 Bruxism (Clenching/Grinding Teeth)
Bruxism (Clenching/Grinding Teeth)
Allergy may play a role in bruxism. It is reported that bruxism is more frequent in those experiencing periods of allergic rhinitis or asthma.
Recommendations for Allergic Rhinitis / Hay Fever:
Amino Acid / Protein
Botanical / Herbal
 Goldenseal
Goldenseal
Golden Seal has antibiotic properties and is helpful in all types of airborne allergy responses such as prevention of hay fever. It is anti-inflammatory to the mucous membranes, and helps reduce and soothe swollen, irritated tissues.
 Echinacea (Coneflower)
Echinacea (Coneflower)
A tincture of equal parts of coneflower (Echinacea), goldenseal (Hydrastis canadensis), cleavers (Gallium asparine), eyebright (Euphrasia officinalis), ginger root (Zingiber officinalis), and elderberry (Sambucus nigra) will strengthen your immune system, increase circulation, and help your respiratory system work better. Take 30 drops two or three times per day.
 Stinging Nettle
Stinging Nettle
Nettles are traditionally used for hay fever and may be drunk as an infusion, 2 cups a day.
 Eyebright
Eyebright
Eyebright is both astringent and anti-inflammatory, and decreases the hypersensitive response of the mucous membranes in the eyes, nose, throat, and ears, thereby reducing and soothing swollen, irritated tissues.
 Elderberry / Sambucol
Elderberry / Sambucol
Elderberry is rich in Vitamin C and the bioflavonoid quercetin, both of which are powerful antioxidants and anti-histamine nutrients. It also helps to reduce mast cell histamine response and reduce mucosa inflammation.
 Picrorhiza
Picrorhiza
[Dorsch W, Stuppner H, Wagner H, et al. Antiasthmatic effects of Picrorhiza kurroa: Androsin prevents allergen- and PAF-induced bronchial obstruction in guinea pigs. Int Arch Allergy Appl Immunol 1991;95: pp.128-33]
Chinese Medicine
 Acupuncture
Acupuncture
Treatment with acupuncture can help promote both immune system function and drainage of lymphatic fluid.
Diet
 Increased Water Consumption
Increased Water Consumption
Dehydration causes the body to produce more histamine, which in turn can cause strong hay fever symptoms. Increased water consumption can help prevent dehydration and clear the nasal passage.
 Increased Fruit/Vegetable Consumption
Increased Fruit/Vegetable Consumption
Fresh fruits and vegetables, whole grains, nuts, seeds, plenty of water and fresh juices are all recommended.
 Animal/Saturated Fats Avoidance
Animal/Saturated Fats Avoidance
Do not eat foods that trigger your allergies: eat fewer foods and additives that are likely to cause inflammation and allergic reactions, such as saturated fats (meats and dairy products), refined foods, eggs, citrus, bananas, chocolate, peanuts, shellfish, food coloring, preservatives, caffeine, alcohol, tobacco, and sugar.
 Plant-Based Nutrition
Plant-Based Nutrition
Many of the diet and lifestyle changes recommended against allergies are a natural consequence of adhering to a more animal-free lifestyle: avoiding saturated fats (meats and dairy products), eggs, shellfish; consuming fresh fruits and vegetables (be careful of citrus in particular though), whole grains, nuts, seeds, and fresh juices; using synthetic materials such as acrylic instead of animal products such as wool.
Drug
 Antihistamines
Antihistamines
Antihistamines, commonly available as sprays or tablets, stop the release of the chemical histamine released by the immune system. They usually effectively relieve symptoms of runny nose, itching, and sneezing.
 Conventional Drug Use
Conventional Drug Use
Over-the-Counter Drugs:
Antihistamines may cause drowsiness. Alpha-adrenergic topical sprays reduce congestion but there is a rebound effect if used for more than a few days. Cromolyn sodium is the only preventative drug choice; works as well as antihistamines but does not cause drowsiness; take continuously or it will not work effectively; it is virtually without side-effects.
Prescription Drugs:
Nonsedating antihistamines may cause life-threatening irregular heartbeat and should not be taken with other drugs or if you have other liver or heart problems. Oral decongestants may have systemic side-effects. Nasal corticosteroid sprays are effective if used properly; improvement takes 1 to 2 weeks. Systemic steroids are prescribed only for severe allergic rhinitis; generally prescribed for short amounts of time because of their many side-effects.
NOTE: Extended use of antihistamines or nasal sprays can make your allergic rhinitis worse.
Environmental
Habits
Homeopathy
 Homeopathic Remedies
Homeopathic Remedies
Dosage is usually 12X to 30C every one to four hours until your symptoms get better. Some of the most common remedies used for allergic rhinitis are:-
- Allium cepa for a lot of irritating nasal discharge and tearing eyes
- Euphrasia for bland nasal discharge, with stinging, irritating tears
- Sabadilla for sneezing with watery discharge from nose and eyes
- Wyethia for an itchy nose, throat, and soft palate.
Laboratory Testing
Mineral
 MSM (Methyl Sulfonyl Methane)
MSM (Methyl Sulfonyl Methane)
Symptoms of pollen allergy may be reduced with MSM supplements. Dr. Stanley Jacobs, author of The Miracle of MSM admits that he does not understand why MSM would help relieve allergies, but he suspects that MSM blocks cell receptor sites for histamine, which triggers allergic symptoms. It is best taken in the evening, a couple of grams per day, perhaps more when the pollen count is high.
Oxygen/Oxidative Therapies
 Ozone / Oxidative Therapy
Ozone / Oxidative Therapy
Many allergy sufferers claim that Hyperbaric Oxygen Therapy (HBOT) greatly relieves their allergy symptoms. The high levels of oxygen provided by this treatment promote optimal functioning at the cellular level, reducing the inflammatory process and allowing the body to heal itself. Preliminary studies have also shown that levels of IgE (the antibody that leads to an immune response) are decreased by HBOT, which may reduce the magnitude of the allergic response. More research is needed.
Physical Medicine
 Topical Applications
Topical Applications
A saltwater nasal rinse will flush out pollen and other irritants, shrink your sinus membranes and increases drainage. Use a nasal rinse made with water and salt to taste like tears. Rinse each nostril and, with your head over a sink, hold your head sideways and let the water run from your upper nostril to your lower nostril. Keep your nostrils lower than your throat to prevent the salt water from draining into the back of your throat.
Vitamins
 Bioflavonoids
Bioflavonoids
Plants high in bioflavonoids such as quercetin and curcuma (rose hips, bilberry) are especially useful because they reduce your body's production of histamines or leukotrienes (substances that cause allergy symptoms) and strengthen connective tissue.
Quercetin appears to stabilize the membranes of the mast cells that release histamine. Since quercetin's action is preventive, it is best taken daily a week or two before pollen season and continued throughout.
 Vitamin B5 (Pantothenic Acid)
Vitamin B5 (Pantothenic Acid)
Pantothenic acid supplementation may reduce allergic reactions, especially allergic rhinitis. One trial on over 100 patients with allergic rhinitis given 250mg of pantothenic acid twice daily found that the majority had almost instant relief. [Martin W. On treating allergic disorders. Townsend Letter for Doctors Aug/Sept 1991: pp.670-1]
Clinical observation: A physician with allergies took 100mg at bedtime and found that his nasal stuffiness cleared in less than 15 minutes and that he stopped awakening at 4 or 5 AM with cough and mucous secretion. He subsequently found that many of his patients also noted significant relief of nasal congestion from supplementation. [Crook WG. Ann Allergy 49: pp.45-46, 1987]
Clinical observation: Observations made in our laboratory indicated that pantothenic acid at about 500mg daily could be used to combat allergy. Subsequently a pharmaceutical house found that, while it was somewhat effective, it was not superior to certain available antihistaminics. [Williams RJ. The expanding horizon in nutrition. Texas Rep Biol Med 19[2]: pp.245-58, 1961]
Note: Pantothenic acid is quite effective in treating nasal congestion caused by allergy. However, if the dosage is too high, it can cause nasal dryness and pruritus. [Roger Williams, U. of Texas at Austin, personal communication to Wayne Martin, quoted in Martin W. Pantothenic acid for allergies. Townsend Letter for Doctors & Patients June, 1997: p.108]
Szorady conducted allergy skin tests on 24 children injecting them with histamine. Pantothenic acid reduced the intensity of skin reaction by 20-50% in all children. [Marz, p.209, 1997]
 Vitamin C (Ascorbic Acid)
Vitamin C (Ascorbic Acid)
Vitamin C is a powerful antioxidant and anti-histamine nutrient. It prevents histamine chemical release and helps in reducing inflammation.
 Vitamin B6 (Pyridoxine)
Vitamin B6 (Pyridoxine)
One older study reported that L-tyrosine (200mg), vitamin B6 (2.5mg) and niacinamide (10mg) when given in combination for the treatment of hay fever, hives, allergic headaches and poison oak dermatitis produced significant symptomatic relief when 1-3 tablets were taken four times/day in milder cases and up to 6 tablets 4-6 times/day in more severe cases. In some cases characterized by more chronic disorders, such as chronic sinusitis, a worsening of symptoms often occurred during the first few days of treatment. This study found that treatment with each the nutrients individually, or with any two in combination, was ineffective. [Widmann RR, Keye JD Epinephrine precursors an control of allergy. Northwest Med 1952:51: pp.588-90]
 Vitamin A
Vitamin A
The following vitamins can help your symptoms: vitamin A (10,000 to 15,000 IU per day); vitamin B6 (50 to 100mg per day); vitamin B5 (50 to 75mg per day); vitamin C (1,000mg three to four times per day); vitamin E (400 IU per day).
Click to see sample report
Your body is a highly complex, interconnected system. Instead of guessing at what might be wrong, let us help you discover what is really going on inside your body based on the many clues it is giving.
Our multiple symptom checker provides in-depth health analysis by The Analyst™ with full explanations, recommendations and (optionally) doctors available for case review and answering your specific questions.
KEY












