Dyspepsia / Poor Digestion: Overview
Alternative names: Dyspepsia, indigestion, heartburn, hyperacidity, stomachache
Indigestion is defined as pain or discomfort in the stomach that is associated with difficulty digesting food. It is often a sign of underlying disease.
- let The Analyst™ find what's wrong
- have a doctor review your case (optional)
- learn what you should be doing right now
Indigestion is a vague problem that is functional in nature and usually not due to an underlying structural cause. Belching, distension and abdominal sounds often occur in association with abdominal or epigastric pain. Because similar symptoms may be due to more serious conditions, it is important to have an accurate diagnosis.
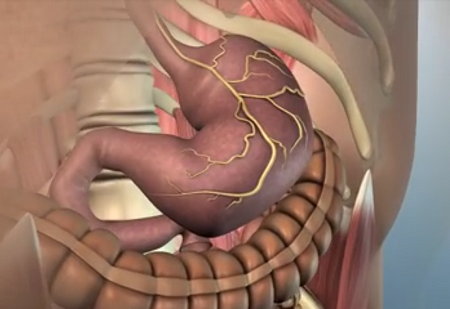
The upper GI tract consists of the organs where food is initially taken into the body and digestion begins, including the esophagus, stomach, pylorus and duodenum.
Aside from indigestion, numerous other conditions are possible in this area, some of which may cause, be caused by, or be mistaken for, indigestion. These include:
- Cardiospasm: Dilation of the esophagus due to the gastroesophageal sphincter failing to open properly and allow food into the stomach.
- Gastroesophageal Reflux Disease (GERD): Incompetent cardiac sphincter, causing backward flow of acid from the stomach up into the esophagus.
- Gastric Mucosal Tears: Lacerations in the mucosa of the gastroesophageal junction, where the esophagus passes through the diaphragm, or in the lining of the lower esophagus. Generally caused by repeated vomiting or retching (repetitive contractions of the abdominal muscles), it can cause profuse hemorrhaging.
- Esophageal Stricture: Narrowing of the esophagus due to scar tissue, resulting in difficulty swallowing.
- Esophageal Obstruction: Blockage of the esophagus caused by tumors or other foreign bodies such as improperly chewed food (often large pieces of meat) impacted in the lower esophagus.
- Esophageal Varices: Enlarged veins in the lower esophagus are a common complication of liver cirrhosis. If these veins rupture, massive bleeding may result.
- Hiatal Hernia: Movement of the upper part of the stomach up into the chest cavity resulting in retention of acid and other stomach contents which can then easily reflux into the lower esophagus.
- Dumping Syndrome: Rapid gastric emptying caused by the lower end of the small intestine (jejunum) filling too quickly with undigested food from the stomach. Symptoms include nausea, vomiting, diarrhea, bloating, shortness of breath, weakness, and dizziness. Stomach surgery is the main cause.
- Hypochlorhydria and achlorhydria: Insufficient stomach acid to sterilize the stomach and start protein digestion.
- Menetrier's Disease: A chronic condition with an unknown cause. Giant folds of tissue, possibly inflamed or containing ulcers, grow in the wall of the stomach and can interfere with the body's absorption of some proteins.
- Whipple's Disease: A malabsorption disease caused by bacteria. Although it can affect any system of the body, it usually attacks the small intestine. It interferes with the body's ability to absorb certain nutrients, causing weight loss, irregular breakdown of carbohydrates and fats, resistance to insulin, and malfunctions of the immune system. The disease can be cured, but if not recognized, it is usually fatal.
- Zollinger-Ellison Syndrome: Another disease of unknown cause leading to gastrin-secreting tumors in the pancreas, which promote an extreme form of peptic ulcer disease in both the stomach and duodenum.
- Peptic Ulcer Disease (PUD): Over 20 million Americans will suffer from a peptic ulcer in their lifetime.
Causes and Development
Indigestion is usually related to eating, which causes the stomach to produce acid and stretch. The most common causes and risk factors include:
- GERD (Gastro-esophageal reflux disease), in which the lower esophageal sphincter (LES) – the muscular ring between the esophagus and the stomach – is unable to prevent stomach acid from rising up into the esophagus
- Smoking – Some of the chemicals in tobacco smoke can relax the LES and allow stomach acid to escape from the stomach
- Alcohol in excess can cause the stomach to produce more acid than it normally does
- Certain medications can also relax the LES, or affect the digestive tract in other ways
- Obesity – Increased pressure inside the stomach, including after a large meal, can cause acid reflux
- Pregnancy – Hormonal changes, as well as increased pressure on the stomach, can cause indigestion
- Stress or anxiety
- Hiatal hernia, in which some of the stomach pushes through the diaphragm and into the chest cavity, which increases risk of regurgitation or acid reflux
- Helicobacter pylori (H. pylori) infection – This bacterial infection can cause stomach ulcers and indigestion
- Stomach ulcers
- Stomach cancer
Signs and Symptoms
Symptoms (see below) usually occur soon after eating or drinking, but there can be a delay between eating and getting indigestion.
Diagnosis and Tests
When diagnosing possible indigestion, it is important to first understand the patient's symptoms, eating and drinking habits, and medicine use. A physical exam would then look for bloating, abdominal sounds, tenderness, pain, or lumps.
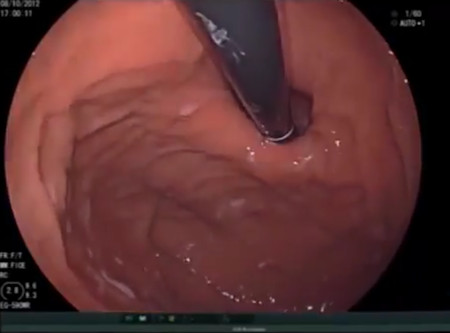
If a problem is suspected in the upper gastrointestinal (GI) tract, an endoscopy may be performed in order to see what is taking place inside. This involves passing a flexible tube with a camera at the end through the mouth and into the upper GI tract.
It is important to determine the cause of indigestion so that it – and therefore also the indigestion – can be treated. An upper GI endoscopy can detect conditions such as gastritis, gastroesophageal reflux disease (GERD), peptic ulcer disease, stomach cancer, narrowing of the esophagus, blockages, and so on.
Certain conditions require that a small sample of tissue be taken and examined to confirm diagnosis. This procedure, known as a biopsy, is done by passing a small instrument through the endoscope.
Other tests include imaging (X-ray, CT scan or ultrasound) and testing for H. pylori infection by using a blood test, stool antigen test, urea breath test, or an upper GI biopsy.
Treatment and Prevention
Treatment of indigestion depends on its cause and severity. Dietary factors are often important in reducing symptoms, and diet/lifestyle changes may be all that is needed: losing weight, exercising, healthy diet, smaller meals, avoiding rich, spicy or fatty foods, avoiding caffeine and alcohol, and stopping smoking.
Going to bed with a full stomach increases risk of indigestion, so eating earlier can reduce risk. Sleeping on a sloping bed, with head and chest slightly elevated, can also help keep stomach acid in the stomach.
Antacids provide immediate relief by neutralizing stomach acid and come in tablet or liquid form.
Proton pump inhibitors (PPIs) restrict the amount of acid produced in the stomach.
Alginates (which form a foam barrier above the stomach acid) and H2-receptor antagonists (which reduce stomach acidity) are other options.
If the cause of indigestion is H. pylori infection, then simple antibiotic treatment is available.
Complications
Severe and chronic indigestion can lead to esophageal stricture, pyloric stenosis, or Barrett's esophagus – a pre-cancerous condition.
On This Page
Poor Digestion:Signs, symptoms & indicators of Dyspepsia / Poor Digestion:
Symptoms - Abdomen
Symptoms - Bowel Movements
Symptoms - Food - Preferences
Symptoms - Gas-Int - General
Symptoms - Head - Mouth/Oral
Symptoms - Nails
Conditions that suggest Dyspepsia / Poor Digestion:
Circulation
Digestion
Infections
 Blastocystosis (Blastocystis hominis)
Blastocystosis (Blastocystis hominis)
In a person with weakened digestion or weakened immune response, blastocystis can produce a host of symptoms which appear to come and go and are very unpredictable.
Metabolic
Skin-Hair-Nails
 Psoriasis
Psoriasis
Incomplete protein digestion or poor intestinal absorption of protein breakdown products can result in elevated levels of amino acids and polypeptides in the bowel. These are metabolized by bowel bacteria into several toxic compounds. The toxic metabolites of the amino acids arginine and ornithine are known as polyamines (e.g., putrescine, spermidine, and cadaverine) and have been shown to be increased in individuals with psoriasis. Polyamines contribute to the excessive rate of cell proliferation. Lowered skin and urinary levels of polyamines are associated with clinical improvement in psoriasis, so digestive function should be evaluated.
Risk factors for Dyspepsia / Poor Digestion:
Digestion
Environment / Toxicity
 Fluoride Toxicity
Fluoride Toxicity
Studies have shown that ingested fluoride damages gastroduodenal mucosa. Gastrointestinal discomfort can be an early warning sign of fluorosis, so fluoride toxicity should be considered a possible reason for non-ulcer dyspepsia and gastrointestinal discomfort in the form of dyspeptic symptoms should be an important diagnostic feature when identifying fluorosis patients and should not be dismissed as non-specific. [Susheela AK, Das TK, Gupta IP, Tandon RK, Kacker SK, Ghosh P, and Deka, Fluoride ingestion and its correlation with gastrointestinal discomfort, Fluoride, 1992, 25:l, pp.5-22]
The gastro-intestinal system is one of the most sensitive systems in the body to react adversely to fluoride toxicity. There are now many case histories available to establish the correlation of fluoride toxicity to gastro-intestinal problems.
Organ Health
Symptoms - Food - Preferences
Dyspepsia / Poor Digestion suggests the following may be present:
Circulation
Recommendations for Dyspepsia / Poor Digestion:
Botanical / Herbal
 Cayenne Pepper
Cayenne Pepper
Although a few sources have recommended cayenne pepper as a potential treatment for dyspepsia, gastritis and even peptic ulcers, most modern herbal texts suggest avoiding the herb for persons with these conditions. A small clinical trial suggests that cayenne may be beneficial in some persons with functional dyspepsia. Approximately 850mg of cayenne powder in a capsule was given 3 times per day just before meals (0.7mg capsaicin per gram). [NEJM 2002;346: pp.947-48]
Diet
 Therapeutic Fasting
Therapeutic Fasting
Fasting gives the digestive system a much-needed rest. After fasting, both digestion and elimination are invigorated.
 Reduced Water Consumption
Reduced Water Consumption
Although dyspepsia is a sign of dehydration, it is generally recommended that you do not drink during a substantial meal, or from 1⁄2 hour before to 2 hours afterwards.
Digestive Aids
 Hydrochloric Acid (Trial)
Hydrochloric Acid (Trial)
Upper digestive symptoms are often due to hydrochloric acid (HCl) or pancreatic insufficiency and it can be difficult to distinguish between the two. The easiest way to find out is to do both an HCl and digestive enzyme trial, one at a time. Often a doctor's assistance is helpful in conducting these trials.
Click to see sample report
Your body is a highly complex, interconnected system. Instead of guessing at what might be wrong, let us help you discover what is really going on inside your body based on the many clues it is giving.
Our multiple symptom checker provides in-depth health analysis by The Analyst™ with full explanations, recommendations and (optionally) doctors available for case review and answering your specific questions.
KEY










