Stroke: Overview
Alternative names: Brain attack
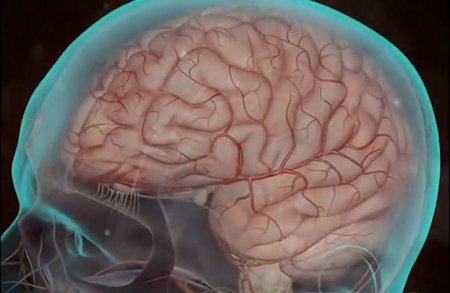
A stroke occurs when brain cells are deprived of their blood supply. Without access to vital nutrients and oxygen, brain cells in the affected area die. The effects of a stroke can vary widely depending on where it occurs in the brain, the severity of the attack, and the general health of the person. A minor stroke may not even be noticed, while a major stroke can cause crippling mental and physical disabilities or even death.
- check your overall health status
- identify any nutritional deficiencies
- learn what you should be doing right now
The brain controls every part the body and all processes taking place within it. Because stroke can occur anywhere in the brain, it means that any part of the body and any bodily function can be affected. One person may develop speaking difficulty; another may no longer be able to walk; another may lose the use of his left arm; another may go blind.
Approximately 75-80% of strokes are of the clotting (ischemic) variety, while the remainder (hemorrhagic strokes) are due to bleeding from broken blood vessels. Sometimes platelets (cells in the blood stream responsible for clotting) become 'sticky' and promote clotting. If the blood clots too easily it can result in blood flow blockage and subsequent tissue death in that part of the brain normally nourished by the affected blood vessel. You can reduce the risk of the blockage type strokes by keeping your blood platelets from becoming sticky.
A completed stroke is caused by irreversible brain injury due to the interruption of blood flow. In contrast, a Transient Ischemic Attack (TIA) is a temporary focal neurologic deficit caused by the brief interruption of local cerebral blood flow. Strokes occur in one third of patients who have had a TIA.
The duration of a focal neurologic deficit that leads to cerebral infarction has arbitrarily been determined to be 24 hours or greater. Any focal neurologic deficit that resolves completely within 24 hours is considered a TIA.
Incidence; Causes and Development; Contributing Risk Factors
Stroke is the third leading cause of death in the United States and the primary cause of disabilities in adults. By the start of the 21st century, more than 700,000 Americans were experiencing a stroke each year and more than 167,000 of those were dying. The estimated cost of that to the nation each year was 51.2 billion dollars (and rising).
A stroke occurs when the blood supply to part of the brain is blocked or reduced for any reason:
- a blood clot (ischemic stroke)
- bleeding in the brain due to rupture of a weakened blood vessel (hemorrhagic stroke)
- a narrowing in one of the brain's arteries
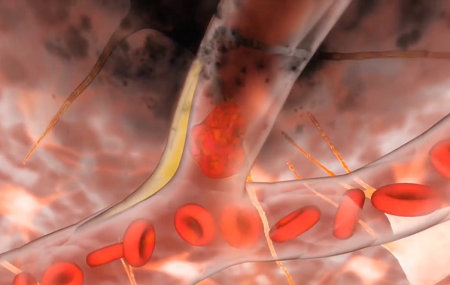
There are two types of ischemic stroke:
- Thrombotic strokes are caused by a blood clot (thrombus) in an artery that supplies blood to the brain. Blood clots usually occur in arteries affected by atherosclerosis – a buildup of hardened plaque on the inner walls. When a plaque ruptures, a blood clot forms at the site of the rupture and blocks the flow of blood.
- Embolic strokes occur when a blood clot (embolus) forms somewhere else in the body, breaks free, and travels to the brain. Eventually the embolus reaches an artery small enough to block its passage.
The interruption in blood supply causes the affected part of the brain to be deprived of oxygen, which after just a few minutes causes some of the brain tissue (brain cells) to die. The more severe the stroke, the more of the brain that is affected.
Elevated blood pressure increases the risk of stroke substantially. Discontinuing hypertensive medication with a return of high blood pressure significantly increases the risk of stroke, especially for someone under the age of 55. Hypertensives are strongly advised not to discontinue medication permanently unless their blood pressure stays close to the normal range.
One study found that while patients on pressure-lowering medications still faced double the stroke risk of healthy controls, patients who abandoned these medications had nearly five times the risk. They authors speculate that the thinning of the arterial wall that occurs with the use of many antihypertensive drugs (due to lowered pressure) might render the wall more subject to injury from high pressure that may occur when medications are ceased. The stroke risk associated with stopping hypertension medication appears to be even higher – almost eight times higher in patients under the age of 55 years than in older patients. This phenomenon might be explained by the vascular thickening that accompanies aging.
Risk factors for stroke include:
- High blood pressure
- Heart disease
- Smoking
- Diabetes
- A history of stroke or TIAs
- History of stroke in the family
- Obesity
- Diets high in alcohol, cholesterol, fat and sodium consumption
- Using oral contraceptives after the age of 35, especially if combined with smoking
- Chronic stress – stress may contribute to maintaining blood pressure at high levels.
Signs and Symptoms
The symptoms of a TIA depend on the region of the brain that is supplied by the transiently occluded cerebral artery. If a TIA is recognized, steps can be taken to prevent future ischemic stroke. All TIAs should be promptly investigated because the risk of ischemic stroke is highest soon after a TIA.
What To Look Out For
During a stroke, parts of your brain are not receiving enough oxygen and this can produce a number of warning signs. These symptoms include:
- A sudden change in your vision, particularly if it occurs in one eye
- Sudden numbness, weakness or paralysis in your leg, arm, or face
- A sudden, severe headache that has no known cause
- A sudden change in your ability to speak or understand speech
- Difficulty standing, unsteadiness, or unexplained dizziness
- Personality changes
- Nausea, vomiting, or drowsiness may also occur during a stroke.
Unfortunately, these symptoms can be permanent.
Diagnosis and Tests
Diagnosis concerning the specific type of stroke, its location, and how severe the damage is, can be determined by using a number of advanced imaging tests including Computerized Tomography (CT) Scans and Magnetic Resonance Imaging (MRI).
The diagnosis of a TIA indicates that no irreversible neurologic injury has occurred and provides an excellent opportunity to prevent permanent damage.
The first step in the evaluation of a patient with possible TIA is to determine if the event in question actually represents a TIA. Certain conditions should be ruled out before the diagnosis of TIA is made. Excluding other diagnoses reduces the possibility of inappropriately labeling a patient with the diagnosis of cerebrovascular disease and launching into a course of costly and potentially dangerous diagnostic testing.
Treatment and Prevention
Treatment and rehabilitation after a stroke may involve work with many health care specialists, including physicians, occupational therapists, physical therapists, nurses, social workers and speech/language specialists. Recovery from a stroke can vary a great deal from person to person. Some people recover in a few weeks, while others may take months or years.
Prognosis; Seek medical attention if...
More than half of men and women under age 65 who have a stroke die within 8 years; long-term survival is worse in men than in women.
A stroke is always a medical emergency, so it is extremely important that you call a doctor or emergency services immediately if you experience any stroke symptoms. Treatments provided within hours of symptoms may help prevent or reduce brain damage. Even if symptoms occur just briefly, and then stop, it is still very important to seek help. These brief symptoms may indicate a TIA (Transient Ischemic Attack) or "mini-stroke" and may be a sign of a serious problem.
Signs, symptoms & indicators of Stroke:
Lab Values - Common
Symptoms - Head - Eyes/Ocular
Symptoms - Head - Mouth/Oral
 Rapid decline in speaking ability
Rapid decline in speaking ability
A mini stroke (TIA) is a brief period of reduced blood flow to an area of the brain, often damaging brain cells and resulting in certain impaired brain functions, such as difficulty speaking.
 Incoherent speech
Incoherent speech
Common signs that a stroke has occurred are difficulty speaking, slurred speech, or garbled speech.
Symptoms - Skeletal
 Slightly/greatly reduced arm function or inability to use arm(s)
Slightly/greatly reduced arm function or inability to use arm(s)
Loss of arm function affects some 85% of those who have suffered a stroke.
Conditions that suggest Stroke:
Lab Values - Common
Mental
 Senile Dementia
Senile Dementia
Multi-infarct dementia is caused by a series of minor strokes. It usually results from damage to the small blood vessels in the brain causing deprivation of blood supply to the brain cells thus affecting its function. Patients' abilities will decline in a step-like pattern.
Risk factors for Stroke:
Addictions
Circulation
 Hypertension (High Blood Pressure)
Hypertension (High Blood Pressure)
High blood pressure is the main risk factor for having a stroke and those with hypertension are 8 times more likely to suffer from stroke than those with normal blood pressure. Long-term high blood pressure narrows and weakens blood vessels, including those in the brain, making it easier for them to rupture or become blocked.
 Hemochromatosis (Iron overload)
Hemochromatosis (Iron overload)
According to a study published in Neurology, high iron levels in stroke patients may prompt more severe neurological symptoms and possibly increase brain damage. Elevations of iron may intensify post-stroke neurological problems such as increased weakness, speech and orientation difficulties, and decreased levels of consciousness. Stroke patients with high ferritin concentrations may also have larger areas of the brain damaged due to stroke. High body iron stores may increase free radical production in brain cells, thus prompting stroke progression.
 Aneurysm / Rupture
Aneurysm / Rupture
Sometimes cerebral aneurysms are the cause of stroke, although most strokes are caused by clotting rather than by a rupturing aneurysm.
Family History
Habits
 Lack of Sleep
Lack of Sleep
If you sleep less than six hours per night and have disturbed sleep you stand a 15% greater chance of developing or dying from a stroke.
Lab Values
 Elevated Homocysteine Levels
Elevated Homocysteine Levels
Stroke risk appears to rise as soon as homocysteine levels reach 7µmol/L, accelerating rapidly as levels rise beyond that.
 Low Total Cholesterol
Low Total Cholesterol
Researchers have found that as cholesterol levels drop, the risk of hemorrhagic stroke (accounting for 20% of strokes) increased significantly. A person with a cholesterol level below 180mg/dl had twice the risk of that type of stroke when compared with someone at a level of 230mg/dl.
Nutrients
 Copper Deficiency
Copper Deficiency
A copper deficiency has been associated with weakening of connective tissue that can be a contributing factor for the development of cerebral aneurysms and hemorrhagic strokes.
 EFA (Essential Fatty Acid) Type 3 Requirement
EFA (Essential Fatty Acid) Type 3 Requirement
Consuming cold water fish (and probably omega-3 fatty acids) reduced the incidence of stroke in women by 28 percent. This study demonstrated a reduction in clotting type strokes, without an increase in hemorrhagic strokes.
Organ Health
 Diabetes Type II
Diabetes Type II
Cardiovascular disease is the leading cause of diabetes-related death. People with diabetes are two to four times more likely to develop cardiovascular disease. At least 65% of people with diabetes die from heart disease or stroke.
Personal Background
 African ethnicity
African ethnicity
The death rate from stroke in African Americans is almost double that of Caucasians.
Sleep
 Obstructive Sleep Apnea (OSA)
Obstructive Sleep Apnea (OSA)
Obstructive sleep apnea (OSA) significantly increases the risk of stroke or death from any cause, and the increase is independent of other risk factors, including hypertension. [N Engl J Med 2005; 353: pp.2034-41]
Another study published April of 2010 in the American Journal of Respiratory and Critical Care Medicine followed 5,422 people aged 40+ who had no history of stroke for 9 years. It was found that even mild OSA led to elevated risk of stroke, and this risk increased with more severe OSA. Men with moderate to severe OSA had 3 times the stroke risk than men with mild or no OSA. The risk in women was also increased, but only in cases of severe OSA.
Supplements, Medications, Drugs
 History of/occasional/regular COX-2 inhibitor use
History of/occasional/regular COX-2 inhibitor use
Animal research suggests that the selectivity of COX-2 inhibitors could create an imbalance that promotes blood clotting and blood vessel constriction. COX-1 makes thromboxane A2, which promotes blood vessel constriction and "stickiness" in blood cells called platelets. COX-2 is the major source of prostacyclin, which helps prevent platelets from clumping and promotes blood vessel dilation. Until further research is completed it may be wise to use COX-2 inhibitors cautiously, if at all, if you are at greater risk of stroke. [Science April 19, 2002;296: pp.539-41]
 Much/some B-complex supplementation
Much/some B-complex supplementation
By reducing levels of homocysteine in the blood, the B vitamins significantly reduce the likelihood of having a stroke.
Symptoms - Cardiovascular
Symptoms - Food - Intake
Symptoms - Muscular
Symptoms - Sleep
 Sleeping more/sleeping less than necessary
Sleeping more/sleeping less than necessary
Several large studies involving hundreds of thousands of people have found that sleeping too much (or too little) increases risk of stroke dramatically. Sleeping 7-8 hours a night and exercising for 30-60 minutes 3 to 6 times per week appears to be optimal for preventing stroke.
 Sleeping less/sleeping more than necessary
Sleeping less/sleeping more than necessary
Getting less than 6 hours of sleep each night increases the risk of early death from stroke.
Stroke suggests the following may be present:
Addictions
 Cigarette Smoke Damage
Cigarette Smoke Damage
Smoking causes cerebrovascular disease primarily by increasing atherosclerosis and thrombosis. Between 50% and 55% of all strokes in the United States are directly attributable to cigarette smoking. A smoker is 1.5 to 3 times more likely to develop cerebrovascular disease.
Stroke could instead be:
Nervous System
 Bell's Palsy
Bell's Palsy
A facial paralysis that has resulted from a stroke is sometimes misdiagnosed as Bell's palsy.
Recommendations for Stroke:
Habits
 Increased Sleep
Increased Sleep
Getting less than six hours' sleep each night doubles the chance of dying from a heart attack or stroke for those at risk.
Preventive measures against Stroke:
Amino Acid / Protein
 L-Taurine
L-Taurine
Taurine reduces platelet aggregation, which is how most natural products work in stroke prevention.
Botanical / Herbal
 Cayenne Pepper
Cayenne Pepper
Cayenne reduces platelet aggregation (makes the blood less likely to clot) and thus may reduce the risk of clotting strokes.
Detoxification
Diet
 Plant-Based Nutrition
Plant-Based Nutrition
A low incidence of cerebrovascular disease was associated with geographical regions where fresh fruit and vegetable consumption (and therefore increased potassium) was high. [Low fruits and vegetables, high-meat diet increase cerebrovascular event risk. Medical Tribune March 10, 1997:26]
 Increased Water Consumption
Increased Water Consumption
A Seventh Day Adventist study found that those who drank 5 glasses of water per day have on average half the cardiac mortality and half the fatal stroke rate of the general population.
 Caffeine/Coffee Avoidance
Caffeine/Coffee Avoidance
Coffee, including decaf, contains significant amounts of Vitamin K which is an important factor for blood coagulation. People at high risk for blood clots, strokes, and heart attacks should avoid coffee and decaf for this reason.
Digestive Aids
 Bromelain
Bromelain
Bromelain is potent enzyme that naturally supports the body's ability to break down blood clots as they develop and diminish inflammation.
Drug
 Aspirin
Aspirin
Aspirin may reduce your chance of having a stroke. Aspirin reduces platelet 'stickiness' or aggregation, as do other natural products that 'thin blood'. The use of aspirin to reduce clotting and stroke risk, even at doses as low as 81mg three times per week, is still controversial. The risks from aspirin are low at the lowest doses, but the benefit may be limited. Aspirin seems to work better in men with low blood pressure than high, and in men who have had a previous heart attack compared to those who have not. There are many natural substances that can reduce stroke risk with fewer side-effects.
Hormone
Supplements
 Policosanol/Octacosanol
Policosanol/Octacosanol
Policosanol inhibits the formation of clots, and may work synergistically with aspirin in this respect. 75% of strokes are of the clotting kind. In a comparison of aspirin and policosanol, aspirin was better at reducing one type of platelet aggregation (clumping together of blood cells) but policosanol was better at inhibiting another type. Together, policosanol and aspirin worked better than either alone.
 EPA (eicosapentanoic acid)
EPA (eicosapentanoic acid)
EPA reduces platelet aggregation and thus helps prevent those strokes that are due to an abnormal clotting tendency.
 Essential Fatty Acids
Essential Fatty Acids
High doses of Omega-3 oils reduce platelet aggregation and thus reduce the abnormal clotting tendency which is seen in 75% of strokes.
Vitamins
 Folic Acid
Folic Acid
A study found that people with a dietary intake of at least 300mcg per day of folic acid reduced their risk of stroke and heart disease by 20% and 13% respectively, compared with those who consumed less than 136mcg of folic acid per day.
[Stroke 2002;33: pp.1183-9]
 Vitamin B6 (Pyridoxine)
Vitamin B6 (Pyridoxine)
Vitamin B6 at 150-200mg daily reduces platelet aggregation, and thus may help prevent ischemic (clotting type) strokes.
Click to see sample report
Your body is a highly complex, interconnected system. Instead of guessing at what might be wrong, let us help you discover what is really going on inside your body based on the many clues it is giving.
Our multiple symptom checker provides in-depth health analysis by The Analyst™ with full explanations, recommendations and (optionally) doctors available for case review and answering your specific questions.
KEY













