Vitamin B12 Requirement: Overview
Alternative names: Cobalamin
Your body needs vitamin B12 in order to create healthy red blood cells; it is absorbed through the intestines from a variety of foods. Because a healthy liver is able to store several years' worth of vitamin B12, signs of deficiency may not be obvious for a long time.
- check your overall health status
- identify any nutritional deficiencies
- have a doctor review your case (optional)
B12 is the largest and most structurally complicated vitamin. It is essential for life, being involved in the metabolism of every cell in the human body. It is needed for:
- Brain function
- Nervous system function
- Red blood cell formation
- DNA synthesis
- Fatty acid and amino acid metabolism
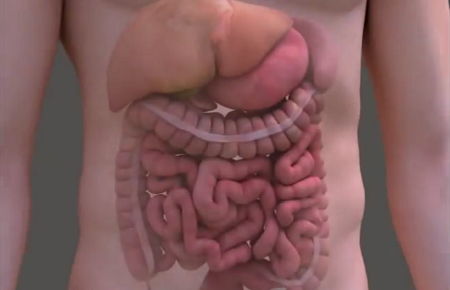
Vitamin B12 can not be absorbed on its own: it must first combine with another substance called 'intrinsic factor' which is produced by your stomach lining. B12 from foods is released from its protein complex by the action of hydrochloric acid and enzymes. The secreted intrinsic factor then binds to B12 and this complex (IF-B12) travels to the end of the small intestine where it crosses the intestinal wall into the bloodstream. B12 is stored in the liver after it is absorbed, and any excess is excreted in the urine. The body contains roughly a 3-year supply and 30% of that found in food is typically destroyed by cooking.
Causes and Development
The most common cause of B12 deficiency the stomach being unable to produce enough intrinsic factor. This is frequently caused by an immune system problem where antibodies attack the stomach lining and damage the cells that produce intrinsic factor.
Another cause is the bowel failing to absorb vitamin B12 because it has been damaged by disease (e.g. Crohn's disease) or shortened by surgery (usually to treat bowel disease). B12 is absorbed by the part of the bowel called the ileum, so surgery to remove the ileum (an ileostomy) is quite likely to cause B12 deficiency.
Although it is also possible to become deficient in B12 by not eating enough food that contains the vitamin, this is rare.
Diagnosis and Tests
A laboratory test can measure the level of vitamin B12 in the blood. A test for low stomach acid (achlorhydria) is an important part of the investigation, and a blood test that shows the typical changes in the red blood cells is also essential.
On This Page
Vitamin B12 Need:Signs, symptoms & indicators of Vitamin B12 Requirement:
Lab Values - Cells
Symptoms - Aging
Symptoms - Bowel Movements
Symptoms - Food - General
Symptoms - Head - Mouth/Oral
Symptoms - Metabolic
Symptoms - Mind - General
Symptoms - Muscular
Symptoms - Nervous
 Numb/burning/tingling extremities
Numb/burning/tingling extremities
If vitamin B12 deficiency becomes pronounced, the nervous system can be affected, causing progressive peripheral neuropathy (tingling of the fingers and toes), muscle weakness, staggering, tenderness in the calves, confusion.
Symptoms - Respiratory
Symptoms - Skeletal
Symptoms - Skin - General
 Lighter/paler skin color
Lighter/paler skin color
Pale skin, often with a lemon tint, can be a sign of vitamin B12 deficiency.
Conditions that suggest Vitamin B12 Requirement:
Circulation
 Megaloblastic Anemia / Pernicious Anemia
Megaloblastic Anemia / Pernicious Anemia
The main indicator of vitamin B12 deficiency is pernicious anemia, which in turn is due to a deficiency of intrinsic factor.
Immunity
Lab Values
Mental
 Depression
Depression
Studies show that one out of four people hospitalized for depression is deficient in pyridoxine and cobalamin.
Musculo-Skeletal
 Osteoporosis - Osteopenia
Osteoporosis - Osteopenia
Researchers at the University of California devised a study to determine if low levels of vitamin B-12 might be associated with bone loss in older women. Results showed that women with the lowest levels of B-12 had a significantly higher risk of bone loss and fractures compared to women with the highest levels. The researchers also noted that for some women, B-12 supplements may help slow the rate of bone loss.
Respiratory
Risk factors for Vitamin B12 Requirement:
Autoimmune
Digestion
Female-Specific
Infections
Lab Values - Nutrients
 Elevated urine MMA levels
Elevated urine MMA levels
The UMMA test is a functional assay. UMMA reflects cobalamin (Vitamin B12) activity at the tissue/cellular level since MMA levels are directly related to a B12-dependent metabolic pathway. The conversion of MMA to succinic acid requires vitamin B12. The metabolic pathway is: MMA → (coenzyme B12 ) → succinic acid.
Vitamin B12 deficiency impedes this pathway and causes MMA levels to increase. Thus, as water builds up behind a dam, high UMMA levels indicate a vitamin B12 deficiency.
 (History of) B12 deficiency
(History of) B12 deficiency
A urine MMA test is recommended for properly diagnosing B12 deficiency due to the possible lack of sensitivity of serum B12 tests.
 Elevated/normal B12 levels
Elevated/normal B12 levels
A normal or high B12 level makes B12 deficiency less likely, but does not rule it out.
Medical Procedures
 Having had a small bowel resection
Having had a small bowel resection
Resection of the bowel increases the risk of vitamin B12 malabsorption. Even 7% to 10% of individuals with serum vitamin B12 levels in the 200-400pg/mL range have developed neuropsychiatric complications of vitamin B12 deficiency. Previously there was only concern when levels were below 200pg/mL.
Organ Health
Parasites
 Tapeworm Infection
Tapeworm Infection
Large parasites like the beef tapeworm compete with us for nutrients by robbing us of micronutrients (such as vitamins) before they get to the things we don't really need.
Supplements, Medications, Drugs
 (Past) H2-blocker antacid use
(Past) H2-blocker antacid use
H2-receptor blockers appear to impair the absorption of vitamin B12 from food. This is thought to occur because the vitamin B12 in food is attached to proteins. Stomach acid separates them and allows the B12 to be absorbed.
 Broad-spectrum antibiotic use
Broad-spectrum antibiotic use
Excessive use of antibiotics or anti-convulsants can lead to B12 deficiency.
Symptoms - Food - Preferences
 Medium-term vegan/long-term vegetarian/vegan diet
Medium-term vegan/long-term vegetarian/vegan diet
Some 80% of those who have been vegan for 2 or more years suffer from some degree of B12 deficiency: B12 deficiency is surprisingly common amongst vegetarians.
 Vegetarian/vegan/raw food diet
Vegetarian/vegan/raw food diet
The authors of one study note that the vegan diet provides essentially no vitamin B12, and people following unsupplemented vegetarian diets may suffer from a deficit as well due to the lower levels in the diet. In addition, people consuming vegan and vegetarian diets were in general also not getting adequate amounts of the essential amino acid methionine, due to the lower methionine content in plant proteins versus animal proteins. [Annals of Nutrition and Metabolism 2000;44: pp.135-8]
Vitamin B12 deficiency is the most common cause of megaloblastic anemia. Both long-term low dietary consumption and poor absorption are responsible for the final outcome of a B12 deficiency, namely megaloblastic anemia and neurological symptoms.
Serum vitamin B12 levels were 37% lower in the vegetarian group and 59% lower in the vegan group, compared with the omnivorous group. Serum B12 levels:
- Vegetarians – 214.8 pmol/l
- Vegans – 140.1 pmol/l
- Omnivores – 344.7 pmol/l
In addition, B12 levels were low enough to be considered clinically deficient in:
- 78% of the vegans
- 26% of the vegetarians
- 0% of the omnivores
Researchers compared homocysteine (Hcy) levels in 62 vegetarians, 32 vegans, and 59 people consuming an omnivorous diet. Compared to the omnivorous group, whose average Hcy levels were about 10.2 mmol/l, levels in the other groups were found to be:
- More than 50% higher in the vegan group (15.8 mmol/l)
- About 30% higher in the vegetarian group (13.2 mmol/l)
Serum folate levels were within the normal range for all three groups, although they were significantly lower in omnivores. The authors conclude that "The results show that the mild hyperhomocysteinemia in alternative nutrition is a consequence of vitamin B12 deficiency."
 Some vitamin B12 supplementation or not supplementing B12
Some vitamin B12 supplementation or not supplementing B12
About 25% of all lacto-ovo vegetarians have a functional B12 deficiency, meaning their homocysteine is too high. The figure is more like 80% for those who have been vegan for 2 or more years. B12 deficiency is very common among vegetarians.
Tumors, Malignant
Recommendations for Vitamin B12 Requirement:
Action
Mineral
Vitamins
 Vitamin B12 (Cobalamine)
Vitamin B12 (Cobalamine)
Treatment is highly effective. The form of vitamin B12 known as hydroxocobalamin is given by injection into a muscle twice during the first week and then weekly until the anemia and all other symptoms of deficiency have been fully corrected. It may be necessary to stay on a maintenance dosage of vitamin B12 every three months for life to stop the problem coming back.
Click to see sample report
Your body is a highly complex, interconnected system. Instead of guessing at what might be wrong, let us help you discover what is really going on inside your body based on the many clues it is giving.
Our multiple symptom checker provides in-depth health analysis by The Analyst™ with full explanations, recommendations and (optionally) doctors available for case review and answering your specific questions.
KEY













