Sinusitis: Overview
Sinusitis is an inflammation of the membranes of the nose and sinus cavity.
- let The Analyst™ find what's wrong
- learn what you should be doing right now
- have a doctor review your case (optional)
Acute sinusitis comes on suddenly and leaves just as suddenly; those with chronic sinusitis have symptoms almost all the time.
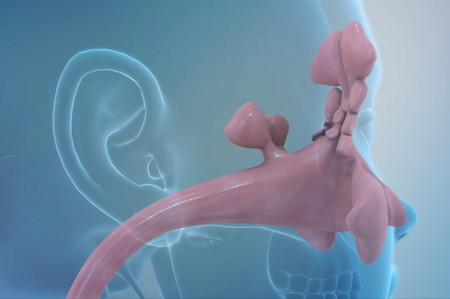
The sinuses are a series of 8 hollow interconnected spaces in the skull. Their walls are lined with mucus-secreting membranes and small hairs that sweep the mucus out of the sinuses so it can drain through the nasal cavity and into the throat.
The two frontal sinuses are located above the eyes; the two maxillary sinuses in the cheeks; the two ethmoid sinuses on either side of the nose between the eyes; and the two sphenoid sinuses behind the eyes.
These mucous membranes may become infected or inflamed because of a cold or allergy and can swell up and block the nasal passages. This is called sinusitis and results in the fluid inside the sinuses being unable to drain, causing pressure, pain and a 'stuffy nose'.
Incidence; Causes and Development
An estimated 37 million people in the U.S. suffer from chronic sinusitis and its incidence has been increasing steadily.
An article published in the Mayo Clinic Proceedings in September, 1999 by the Mayo Clinic suggests that fungal sinusitis may be much more common than previously thought. The disease previously known as AFS (allergic fungal sinusitis) is now know as EFRS (eosinophilic fungal rhinosinusitis) or EMRS (eosinophilic mucinous rhinosinusitis). Fungal growth was found in washings from the sinuses in 96% of patients with chronic sinusitis. Normal controls had almost as much growth, the difference being that those patients with chronic sinusitis had eosinophils (a type of white blood cell involved in allergic and other reactions) which had become activated. As a result of the activation, the eosinophils released a product called MBP (Major Basic Protein) into the mucus which attacks and kills the fungus but is very irritating to the lining of the sinuses. MBP is believed to injure the lining of the sinuses and this in turn allows bacteria to proliferate.
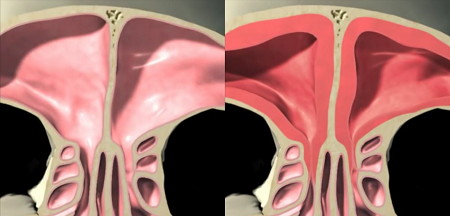
Any factor that creates edema of the nasal tissues resulting in obstruction and the lack of proper drainage of the area will often lead to sinus infection. As the obstruction continues, oxygen is resorbed from the sinus cavity back into the blood vessels, causing a painful relative negative pressure that draws fluid from the mucous membranes. This fluid is an excellent medium for bacteria, especially streptococcus, pneumococcus, haemophilus influenza and staphylococcus, which are the bacteria most implicated in acute sinusitis. The bacterial overgrowth leads to an influx of serum and leukocytes to fight the infection, setting up a painful positive pressure.
Signs and Symptoms
Common symptoms are runny nose, nasal congestion, loss of smell and headaches.
Treatment and Prevention
In cases of acute sinusitis, the therapeutic goals are to reestablish drainage and clear up the infection. Various measures can be used: local application of heat, local use of volatile oils and botanicals with antibacterial properties, and immune system support.
It appears that a key to resolving the problem will be to reduce the immune response or activation of eosinophils to the fungus. Just as one person reacts to ragweed while another does not, reducing the overactivity of the immune system may lead to lower levels of eosinophils (or less activation thereof), less irritation, and fewer symptoms. Since chronic sinusitis is associated with allergy, long-term control can be dependent on isolation and elimination of the food or airborne allergens which may be contributing to the overall allergic load and correction of the underlying problem which allowed the allergy to develop. This may require desensitization procedures. During the acute phase, elimination of the common food allergens (milk, wheat, eggs, citrus, corn, peanuts) is indicated until a more definitive diagnosis can be made.
In 25% of chronic maxillary sinusitis (in the cheek bone area) there is an underlying dental infection which must be resolved.
Although vasoconstrictors and antihistamines cause transient relief, their chronic use is contraindicated, since there is usually a rebound congestion (severe congestion caused by the excessive or abusive use of topical nasal decongestants) following continual administration.
Antibiotics and over-the-counter decongestants are widely used to treat chronic sinusitis. In most cases, antibiotics are not effective for chronic sinusitis because they target bacteria, not fungi. Fungal spores (the reproductive part of the organism) become airborne like pollen. Some people develop allergies to fungi.
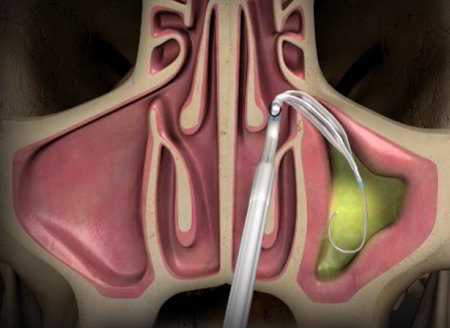
In severe cases, surgical opening of blocked sinus passages may be required. In the past, surgical instruments were used to remove bone and tissue that was preventing sinus drainage. A more recent innovation, called balloon sinuplasty, does not require cutting or tissue removal. A small, flexible balloon catheter is inserted into the blocked passageway and inflated. The passageway is opened up, and the sinus can drain.
Complications
Frequently, the chronic inflammation leads to polyps, small growths in the nasal passages that hinder breathing.
On This Page
Sinusitis:Signs, symptoms & indicators of Sinusitis:
Lab Values - Cells
Symptoms - General
Conditions that suggest Sinusitis:
Circulation
Symptoms - Head - Nose
Recommendations for Sinusitis:
Amino Acid / Protein
Botanical / Herbal
 Cayenne Pepper
Cayenne Pepper
Cayenne may have some supportive activity as an antimicrobial to help control infections such as sinusitis.
Homeopathy
 Euphorbium Nasal Spray
Euphorbium Nasal Spray
German physician Michael Weiser, MD tested Euphorbium Nasal Spray against a placebo on 172 patients. Each patient received 2 discharges of spray into each nostril 4 times a day for 5 months. Patients with chronic sinusitis experienced considerable improvement in terms of reduced headaches, sinus pressure, and breathing difficulties.
Another study conducted by German doctors with 3,510 patients with chronic sinusitis found that 75% rated the nasal spray as "excellent" to "good." Euphorbium Nasal Spray is available in the U.S.
Invasive / Surgery
 Sinus Swabs / Nose Drops
Sinus Swabs / Nose Drops
This treatment has helped many people treat a chronic sinus infection and takes about 6 weeks of self-application.
Laboratory Testing
 Bacteria / Pathogen Testing by PCR
Bacteria / Pathogen Testing by PCR
A Respiratory (Sinusitis/Pneumonia) Panel (Blood or Swab) can test for the presence of Mycoplasma fermentans, Mycoplasma pneumonia, Legionella pneumoniae and Chlamydia pneumoniae.
Mineral
Physical Medicine
Vitamins
 Vitamin B6 (Pyridoxine)
Vitamin B6 (Pyridoxine)
One older study reported that L-tyrosine (200mg), vitamin B6 (2.5mg) and niacinamide (10mg) when given in combination for the treatment of hay fever, hives, allergic headaches and poison oak dermatitis produced significant symptomatic relief when 1-3 tablets were taken four times/day in milder cases and up to 6 tablets 4-6 times/day in more severe cases. In some cases characterized by more chronic disorders, such as chronic sinusitis, a worsening of symptoms often occurred during the first few days of treatment. This study found that treatment with each the nutrients individually, or with any two in combination, was ineffective. [Widmann RR, Keye JD Epinephrine precursors an control of allergy. Northwest Med 1952:51: pp.588-90]
Click to see sample report
Your body is a highly complex, interconnected system. Instead of guessing at what might be wrong, let us help you discover what is really going on inside your body based on the many clues it is giving.
Our multiple symptom checker provides in-depth health analysis by The Analyst™ with full explanations, recommendations and (optionally) doctors available for case review and answering your specific questions.
KEY











