Degenerative Disc Disease
Degenerative Disc Disease (DDD): Overview
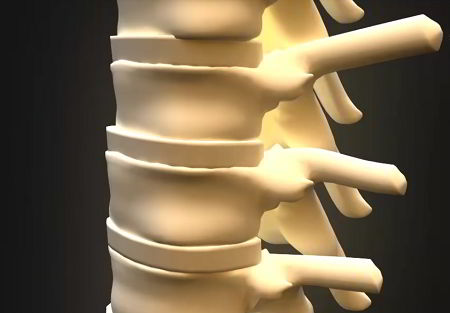
Degenerative Disc Disease is a condition in which the discs between the vertebrae break down, often causing pain and weakness. The affected intervertebral discs shrink in height (collapse) as their annulus (outer shell) weakens and the nucleus (center) gradually loses water; these discs then bulge out into the surrounding spinal canal and can put pressure on any number of spinal nerves.
- let The Analyst™ find what's wrong
- learn what you should be doing right now
- have a doctor review your case (optional)
Intervertebral discs are spongy cushions found between the vertebrae of the spine. These 23 discs have three important functions:
- They are shock absorbers
- They are tough ligaments that help hold the vertebrae of the spine in place
- They are joints that allow the spine to bend and twist
At birth, approximately 80% of each disc is composed of water: a disc needs to be well hydrated in order to function properly. As we age, our discs lose some of this water (dry out), becoming thinner and less 'spongy'.
Degenerative Disc Disease is somewhat of a misnomer. It is in fact not a disease, but simply a natural part of aging in most people, and it is not due to some ongoing degenerative process but simply natural daily movements, continuing stresses (weight gain, heavy lifting, etc.), and minor injuries.
Nevertheless, it is a major concern due to its potential effects on quality of life. Spinal discs degenerate faster than any other connective tissue, due to the extreme stresses put on them.
Incidence; Causes and Development
Approximately 1-in-4 of those aged under 40 already have some disc degeneration; the figure rises to 3-in-5 for those over 40.
There is good evidence – particularly in the case of women (menopause, loss of estrogen) – that sex hormones (estrogen, progesterone, testosterone) play a role in DDD.
Signs and Symptoms

Degenerative disc disease does not always cause symptoms, and symptoms do not necessarily correlate with the amount of damage: The same degree of degeneration in two different people can cause no symptoms in one, but severe chronic pain in the other. When symptoms are present, they include:
- Acute or chronic pain in the affected area, usually low back and/or neck
- Pain that is made worse by movement (sitting, standing up, bending, lifting, twisting)
- Nerve pain depending on the location of the affected discs and the amount of pressure on the surrounding nerves.
Cervical Spine (Neck)
Disc degeneration in the neck often causes pain in the neck, shoulders, arms and hands. If nerves are being compressed, there may also be tingling in the fingers.
Lower Back
A degenerated disc in the lower back can produce lower back pain, extending out to the hips, buttocks, thighs and/or legs. Episodes of tingling or weakness in the knees and legs can also occur if there is pressure on the nerves.
Diagnosis and Tests
Diagnosis generally involves
- Looking for back injuries or stress in the patient's medical history
- A physical exam aimed at detecting muscle weakness, spinal tenderness, and limited range of motion
- An MRI scan to confirm diagnosis and rule out other possible causes of symptoms.
The typical imaging study findings are discs that appear black, disc space narrowing, accumulation of gas ("vacuum disc"), thickening or hardening of the bone ("end plate sclerosis"), and osteophyte (bony outgrowth, bone spur) formation.
Telltale signs of DDD include disc protrusion (bulging discs or herniated discs), spondylolysis (a defect or fracture in one or both of the wing-shaped parts of a vertebra), spondylolisthesis (subluxation/misalignment of the vertebrae), and/or spinal stenosis (growth of bone spurs).
Treatment and Prevention
Nonsurgical treatment for DDD usually consists of a combination of physical therapy, traction, NSAIDs, or epidural steroid injections in order to control the pain. This, however, does nothing to address the underlying problem.
When the consequences of degenerative disc disease are severe, surgery may be the only option. Reasons for surgery include debilitating pain, weakness or numbness in the legs, and impaired walking or standing.
The most common form of surgical treatment for DDD is spinal fusion, where two or more vertebrae are joined together. However, there are at least a dozen other types of surgical treatment available, involving procedures such as (from least to most invasive):
- decompressing the spine to help the spinal discs rehydrate
- reducing a disc bulge by using a needle to remove material
- using heat to seal a disk and deaden nerves
- removing part of a herniated disc nucleus using a surgical instrument or laser
- replacing degenerated intervertebral discs with artificial discs
- replacing an intervertebral disc with a small plug of bone
- rerouting pressure on a disc through the rear of the spinal column
- removing a small part of a vertebra to relieve pressure on nerve roots
- removing a part of a facet joint, or vertebra and surrounding discs, to decompress the spinal cord
- enlarging or reconstructing the spinal canal (nerve pathway) to make more room for the spinal cord
Prognosis; Complications
While it causes no problems for some people, degenerative disc disease can lead to chronic disability and loss of quality of life in others.
As water is lost from the spinal discs, they gradually become thinner and less flexible. Their outer layers are then at increased risk of cracking or tearing and, with enough pressure, the center of the disc (nucleus pulposus) can leak out through these tears and cause a herniated disc.
As the discs collapse and the vertebrae move closer together, the facet joints along the back of the spine are forced to shift, which can affect the way they work. (This disc collapse also partially explains the decrease in height that most humans experience as they age.)
A further consequence of DDD is the formation of bone spurs which grow around the disc space as a way for the body to prevent excessive movement. If these bone spurs grow into the spinal canal, they can put pressure on the spinal cord and surrounding nerves – a condition called Spinal Stenosis.
The alignment of the spine may deteriorate, and the patient may tilt forward due to the collapsed disc(s).