Neck Arthritis: Overview
Alternative names: Cervical arthritis, Cervical osteoarthritis, Cervical spondylosis
Arthritis in the neck, known as Cervical Arthritis, is an osteoarthritic condition affecting the upper spine. The vertebrae in the neck, known anatomically as the cervical vertebrae, begin to degenerate, accompanied by degeneration in the flexible disks of shock-absorbing cartilage that fit between them. These changes gradually narrow the space in the vertebra called the foramen. This narrowing causes compression on the nerves leading from the spinal cord in the neck; the nerves become inflamed, producing pain in the neck that may radiate to the arms.
- see your health summarized and in detail
- understand what's happening to your body
- identify any nutritional deficiencies
Your spine, or backbone, consists of the column of 33 bones and tissue that extends from your skull down to your pelvis. Providing the support of your head and body, your backbone encloses and protects a cylinder of nerve tissues, called the spinal cord.
The 33 bones in your spine are called vertebrae (one is called a vertebra). The upper 24 vertebrae join together like links in a chain. In between each vertebra is an intervertebral disc, a band of cartilage that acts as a shock absorber between the vertebrae. When someone has a "slipped disc," he or she has an intervertebral disc that has slipped out of position, thus causing friction between two vertebrae and extreme pain from nerves being exposed. The lowest nine vertebrae are fused (joined) together in two groups, forming the sacrum and coccyx.
The cervical vertebrae (numbered C1 through C7 from top to bottom) are the seven vertebrae in your neck that form the upper part of your spine, between the skull and the chest.
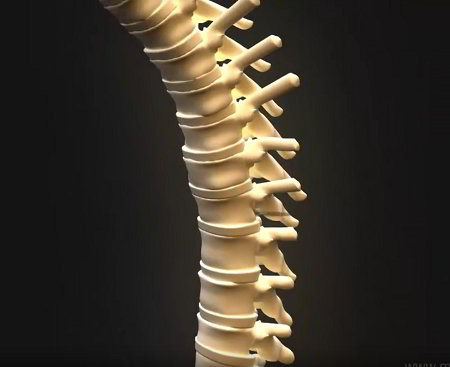
The thoracic vertebrae (numbered T1 through T12 from top to bottom) are the 12 bones between your neck and your lower back. Thoracic vertebrae have cup-shaped surfaces called facets, in which the ribs rest and connect to the spine. These 'joints' help the ribs to move up and down during breathing.
The lumbar vertebrae (numbered L1 through L5 from top to bottom) are the five largest and strongest vertebrae. They are found in your lower back between the chest and hips. The strong muscles of the back are attached to the lumbar vertebrae.
Your sacrum and coccyx are the bones found at the base of your spine. The triangular sacrum – usually made up of five vertebrae (S1 through S5) fused together, but possibly only four – supports the spine and connects it to the pelvis. Your coccyx, or tailbone, is usually formed from four fused vertebrae (Cx1 through Cx4), but possibly three or five, and has little function.
The vertebral foramen is the hollow part of the vertebrae where the spinal chord (nerve tissues) attaches to your brain and sends signals all over your body.
Incidence; Causes and Development
Cervical arthritis tends to begin between the ages of 30 and 50 as part of the normal aging process; like all arthritic conditions, it may grow worse over time. Nearly everyone over the age of 50 experiences some wear and tear in the cervical spine, but not everyone develops symptoms of cervical arthritis.
Once the cervical vertebrae and their disks begin to degenerate, a minor injury to the spine (such as that caused by a fall or sudden twist) may provoke symptoms. This condition may also begin earlier in life, perhaps as the result of a back injury, such as those experienced while playing football or falling from a horse.
Signs and Symptoms
While cervical arthritis tends to affect men more often than women, its symptoms may be similar to those produced by two conditions seen more frequently in women: rheumatoid arthritis and osteoporosis. Symptoms of cervical arthritis may include:
- Chronic neck pain, particularly with motion
- Muscle weakness, with numbness in the neck and arms, perhaps also the hands and fingers
- Tenderness to the touch at the neck itself
- Stiffness which limits movement of the neck
- Headaches
- Loss of Balance.
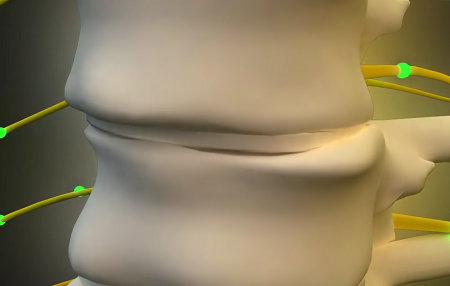
Degeneration of the cervical vertebrae can produce several different conditions affecting the spinal cord and nerve roots. Bony ridges, called osteophytes, often develop on the vertebrae as a result of arthritic change, reducing space for the spinal cord and limiting movement of the neck. The facets of the vertebrae (those portions that interlock with each other, forming joints in the structure of the spine) may also show wear and tear.
Occasionally one of the soft disks cushioning the vertebrae may rupture, resulting in a herniated disk. When this happens, there is usually pressure against the spinal cord or nerve roots also. A herniated disk is a distinct problem, however, usually occurring as a single instance, whereas cervical arthritis is a progressive, chronic process that waxes and wanes over time. Cervical disc hernias usually result in prominent arm and hand pain rather than neck pain.
About 5-10% of patients who have symptomatic cervical arthritis develop myelopathy, or compression of the long tracts of the spinal cord. This may produce symptoms of weakness and spasticity, loss of sensation or of one's sense of position in space, and incontinence. As strange as it may seem, neck and radiating nerve pain is unusual in these cases.
Diagnosis and Tests
If you experience chronic neck pain, your doctor may use a number of different tests to determine whether your condition is cervical arthritis. X-rays show any abnormalities in the bones of the spine, and help determine the amount of degeneration in the vertebrae and their facets. A myelogram with CT (computer tomography) scan provides the best detail of the bone structure of the spine. MRI (magnetic resonance imaging) scans are sometimes done to get a clearer picture of other structures in the spine besides bone.
If X-rays or other imaging tests show that your particular case of cervical arthritis is severe (as in the case of numbness resulting from a disk pressing onto the nerves), your doctor may refer you to an orthopedic surgeon for further evaluation.
Treatment and Prevention
Because of rapid advances in medical technology during the last several decades, cervical arthritis can now be detected much earlier. This is good news, because arthritic conditions that are detected early can be managed and observed with care. The likelihood of severe disability or sustained neck-shoulder-arm pain secondary to cervical arthritis can be detected much earlier.
Most cases of cervical arthritis respond to conservative treatment that is carefully thought out for each individual. Rest of the neck area is essential. To accomplish this, it may be necessary to consider your general posture, the kinds of pillows you use in bed, and the features of your occupation that affect the condition of your neck.
Non-steroidal anti-inflammatory medications (NSAIDs) such as aspirin, acetaminophen or ibuprofen may be recommended to decrease swelling and relieve pain. Sometimes time-released medication is most effective. While other painkillers may be prescribed, narcotic pain medication is generally avoided.
Patients who have a severe episode of cervical arthritis may benefit from a single treatment of a steroid epidural, injected directly into the affected part of the neck. This form of treatment can often relieve the situation to such a degree that other treatment measures can then be put into place.
Other non-operative measures may include cold compresses to relieve acute pain. Massaging the muscles is also helpful and then avoiding stressful conditions may also help. Your physician may recommend ultrasound or whirlpool treatments. A physical therapist may be able to guide you in performing gentle neck exercises, and will have advice about improving your posture in order to minimize the effects of cervical arthritis.
Positioning of the neck may improve or worsen neck pain. When arthritis is the primary cause of the pain, the neck might be made to feel better in a flexed position. If, on the other hand, this is the result of a motor vehicle injury or a blow, then putting the neck in extension may relieve the pain. Traction is also helpful. A simple method of performing traction is to use the weight of your head as a traction device. If your pain is eased in extension, lying on a bed with your head off the end of the bed, will provide eight pounds of traction. Pillows can be placed underneath the knees to avoid stretch and hyperextension of the low back. If arthritis is the problem and the pain is relieved more with flexion lying on your stomach with a pillow under the pelvis and the ankles with the head dangling off of the bed may be helpful. This provides eight pounds of traction in flexion. Remember however, as this may relieve pain, be careful that you do not fall asleep in this position.
Surgery is generally recommended only in more severe cases of cervical arthritis, when the condition appears unresponsive to other forms of treatment. Patients should discuss the possibility of surgery with an experienced orthopedic surgeon, weighing the likelihood of success in their particular case.
Surgical procedures are tailored to the severity of the condition. Sometimes the surgeon can remove a portion of bone, relieving pressure on the spinal cord. Surgery may also be used to fuse some of the cervical vertebrae, remove a damaged disk, or enlarge the spinal cord space by clearing it of bony spurs. Sometimes bone graft procedures are used.
When surgery for cervical arthritis is performed, in carefully selected patients, improvement is seen 60-84% of the time. When patients are over the age of fifty, with symptoms that have lasted for more than 12 months, surgery is less likely to produce significant improvement. Surgical outcomes are also more complicated when there are multiple levels of degeneration, involving more disks, nerves, and vertebrae.
Some of the potential risks of surgery include:
- injury to nerves and blood vessels
- risks of anesthesia, including death
- excessive bleeding
- blood clots
- infection.
It is important to keep in mind that some degree of cervical spondylosis can be seen in 25-50% of the population over the age of 50 and in 75% of those people who are older than 75. Because most people do not develop chronic debilitating symptoms from this condition, each individual must be assessed carefully to determine which symptoms may be caused by cervical arthritis, and to what degree.
When required, excellent or good results of surgery are more possible now than in the past, due mainly to advances in diagnostic imaging and surgical procedure.
On This Page
Cervical Arthritis:Signs, symptoms & indicators of Neck Arthritis:
Symptoms - Skeletal
KEY







